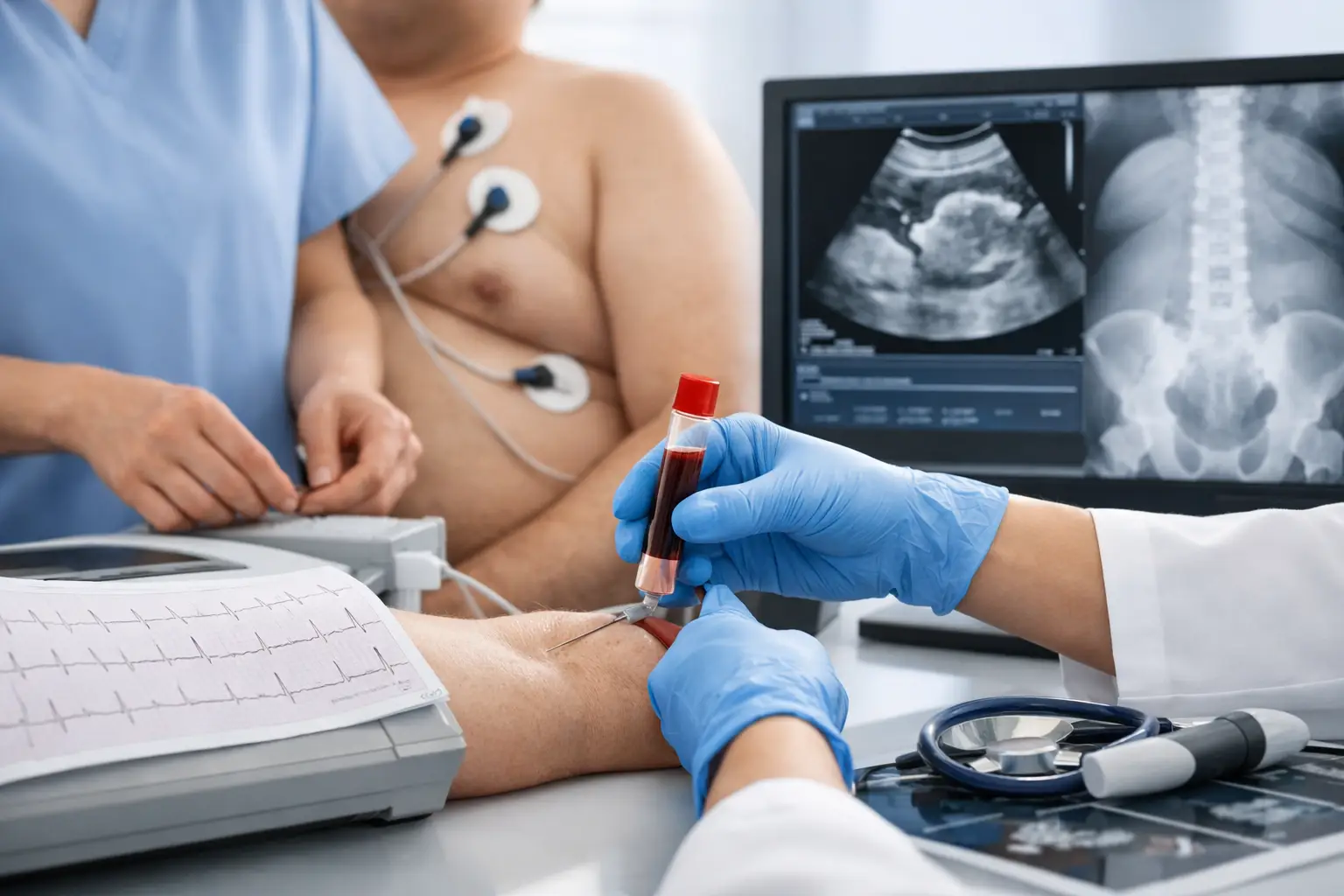
Most patients worry about the operation itself. In reality, a lot of the safety work happens before you ever enter theatre. ECG blood tests imaging before bariatric surgery are there to answer one question clearly: is your body ready for anaesthetic and surgery, and does your surgeon need to plan around anything specific?
That pre-operative stage can feel like a delay when you are eager to move forward, especially if you have been struggling with your weight for years and have finally made a decision. But these checks are not box-ticking. They help the clinical team spot hidden risks, confirm the right procedure pathway, and avoid unpleasant surprises on the day of surgery.
Why ECG blood tests imaging before bariatric surgery matter
Bariatric surgery is carefully planned surgery, not rushed surgery. Even when a patient looks well and feels generally fit, obesity can place extra strain on the heart, lungs, liver and metabolic system. Conditions such as high blood pressure, insulin resistance, sleep apnoea and fatty liver disease are common, and some are not fully obvious without testing.
This is why the pre-op work-up matters so much. It gives the surgeon, anaesthetist and wider hospital team a fuller picture of your health. Sometimes the results simply confirm that everything is straightforward. Sometimes they lead to small changes, such as extra hydration, a medication adjustment, a different anaesthetic plan or a closer post-operative observation period. Those changes can make a real difference to safety and recovery.
For international patients, this stage is also reassuring for another reason. Travelling abroad for surgery can feel daunting if you imagine arriving with unanswered questions. A well-managed pre-op pathway replaces uncertainty with structure.
What an ECG checks before bariatric surgery
An ECG records the electrical activity of your heart. It is quick, painless and usually done in a matter of minutes. Small stickers are placed on the chest and limbs, and the machine records your heart rhythm.
The reason this matters before bariatric surgery is simple. Your heart will need to cope with anaesthetic, fluid shifts and the stress response that comes with any operation. An ECG can help identify rhythm problems, signs of previous cardiac strain, or clues that further review may be needed.
That does not mean an abnormal ECG automatically stops surgery. Quite often it leads to a more detailed assessment rather than a cancellation. It depends on what the tracing shows, your age, your symptoms, your medical history and whether you have known conditions such as hypertension or diabetes. In some patients, the ECG is purely confirmatory. In others, it helps the anaesthetist plan more cautiously.
If you have ever had chest pain, palpitations, breathlessness on exertion or a diagnosed heart condition, tell your coordinator and clinical team early. It is always better for the team to know more, not less.
Blood tests before bariatric surgery
Bloodwork gives a surprisingly detailed snapshot of how your body is functioning. Before bariatric surgery, it is used to check for problems that could affect healing, anaesthetic safety or recovery.
Common blood tests include a full blood count to look for anaemia or infection, kidney and liver function tests, blood glucose or HbA1c to assess diabetes control, clotting studies, thyroid function in some cases, and levels of key nutrients such as iron, vitamin B12, folate and vitamin D. Depending on your history, the team may also request additional tests.
These results matter because bariatric patients do not all start from the same place nutritionally or metabolically. One person may carry excess weight but have normal blood markers. Another may already have low iron, poor glucose control or signs of liver stress. If that second patient goes into surgery without those issues being recognised, recovery can be harder and risks may be higher.
There is also a practical side to this. Blood tests can influence timing. If something mild turns up, the team may still proceed with a simple adjustment or supplement plan. If something more significant appears, surgery may be delayed until it is safer. That can feel frustrating in the moment, but it is a protective decision, not a setback.
What imaging is used before bariatric surgery?
When patients hear “imaging”, they sometimes imagine a long list of scans for everyone. In practice, it depends on the clinic, the surgeon, your medical background and the procedure being planned. Not every patient needs the same imaging before bariatric surgery.
A chest X-ray may be used to assess the heart size and lungs, particularly if there is a respiratory history or anaesthetic concern. An abdominal ultrasound is also common, especially to look at the liver and gallbladder. This is relevant because fatty liver disease is common in bariatric patients, and gallstones may affect planning or post-operative advice.
In selected cases, additional imaging or investigations may be recommended. For example, if you have symptoms of reflux, swallowing difficulty, a previous abdominal operation or suspected hernia, the surgeon may want a closer look before deciding on the most suitable procedure. Revisional bariatric cases usually need more detailed review than first-time surgery because the anatomy and previous surgical changes matter.
This is one of those areas where “it depends” is entirely normal. More tests do not necessarily mean something is wrong. Sometimes they simply mean the team wants a more precise map before operating.
ECG blood tests imaging before bariatric surgery and procedure planning
These checks are not only about deciding whether you are fit for surgery. They also help determine how surgery should be carried out and which option is likely to be the safest and most effective for you.
For instance, blood sugar control may affect peri-operative management. Liver findings on ultrasound may influence surgical difficulty, especially if the liver is enlarged from fatty change. Reflux symptoms combined with other findings may steer discussion away from one procedure and towards another. A heart rhythm issue may shape how the anaesthetic team monitors you before, during and after the operation.
This is why a good bariatric pathway feels coordinated rather than fragmented. The test results need to be seen together, not in isolation. When the surgeon, anaesthetist and support team are all working from the same information, planning becomes safer and smoother.
For many international patients, that joined-up process is just as valuable as the surgery itself. It reduces the stress of trying to interpret medical terms on your own and gives you a clearer sense of what happens next.
What patients can do before pre-op testing
You do not need to prepare in a complicated way, but a few practical steps help. Bring an accurate list of medications, including supplements. Mention any previous operations, allergies, heart or lung conditions, diabetes, CPAP use, blood clot history and smoking status. If you have had recent test results in your home country, those may be useful too, although the treating hospital will still follow its own assessment protocols.
It also helps to be honest about symptoms you might otherwise brush off. Breathlessness, leg swelling, severe reflux, heavy snoring, dizziness or poor exercise tolerance are all relevant. Patients sometimes hold back because they worry surgery will be cancelled. In reality, sharing the full picture gives the team the best chance to manage risk properly.
If fasting instructions are given for blood tests or imaging, follow them carefully. The same goes for any advice on medications. Some treatments should be continued, while others may need temporary adjustment.
If a test result is not normal
This is often the moment anxiety spikes. Patients hear that something needs reviewing and immediately fear the whole plan is collapsing. Usually, that is not what is happening.
A result may be mildly outside the normal range for reasons that are manageable. Sometimes repeat testing is all that is needed. Sometimes the surgeon asks for an additional opinion or a short period of treatment first. And sometimes the team decides to postpone surgery because proceeding would not be in your best interest.
That last scenario can be disappointing, but it is also a sign of a responsible clinical pathway. Safe bariatric care is not about pushing every patient through on the original date. It is about making sound decisions based on real findings.
At Bridge Health Travel, much of the stress reduction comes from having one team help you understand what each stage means, rather than leaving you to work it out alone in a foreign system. That support matters most when plans need adjusting.
The bigger picture behind pre-op checks
Patients often ask whether all this testing means bariatric surgery is especially risky. The fair answer is that every operation carries risk, and bariatric surgery is no exception. But structured pre-op screening is one of the reasons modern bariatric care is much safer than many people assume.
These tests help move the process from guesswork to evidence. They identify what is ordinary for you, what needs attention, and what the team can do to protect you throughout the surgical journey. They also help set expectations for recovery, follow-up and longer-term nutritional care.
If you are at the stage of arranging surgery, try to see ECGs, bloodwork and imaging not as hurdles, but as signs that your care is being taken seriously. A good bariatric experience starts well before the operation, with a team that checks carefully, explains clearly and plans around you.