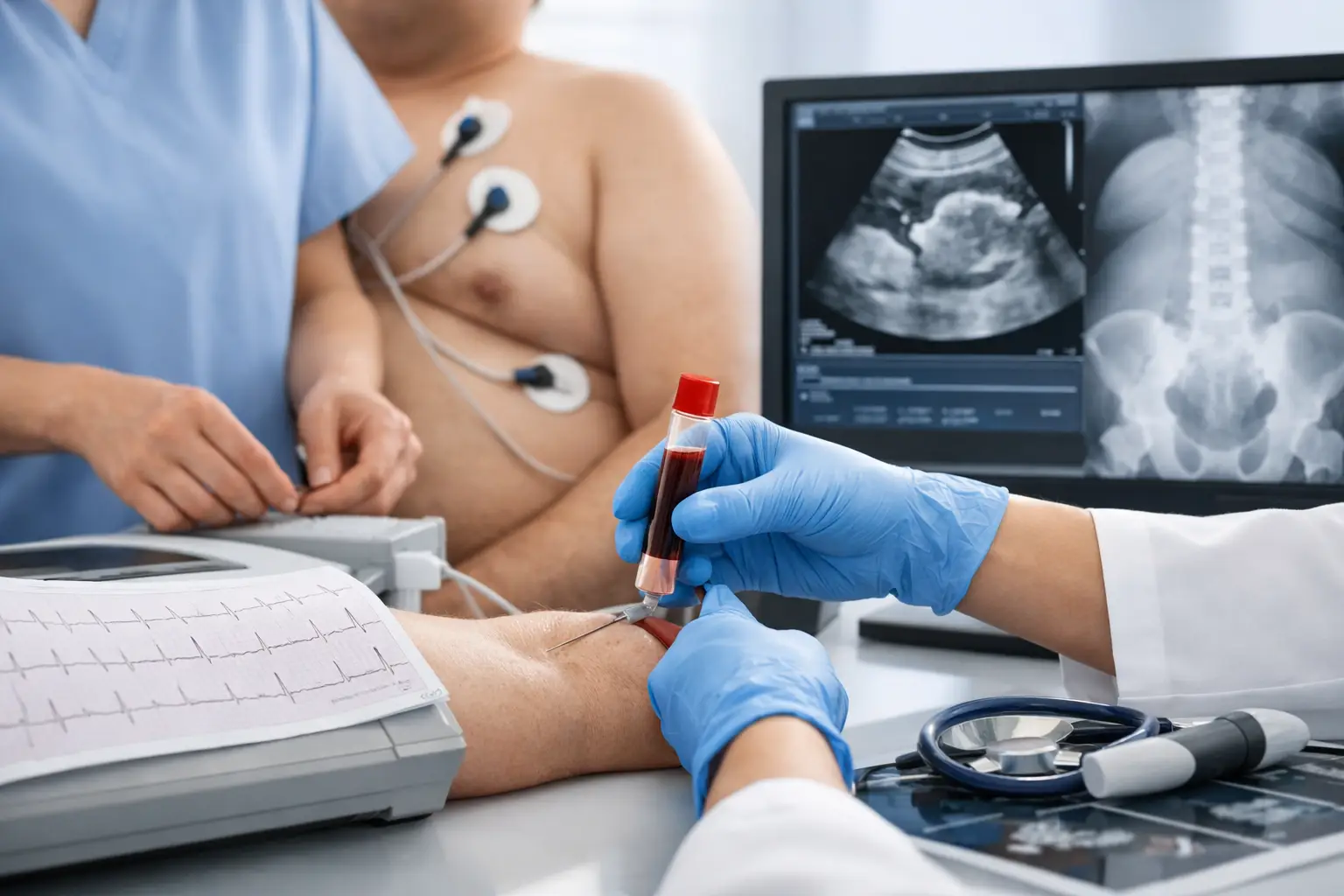
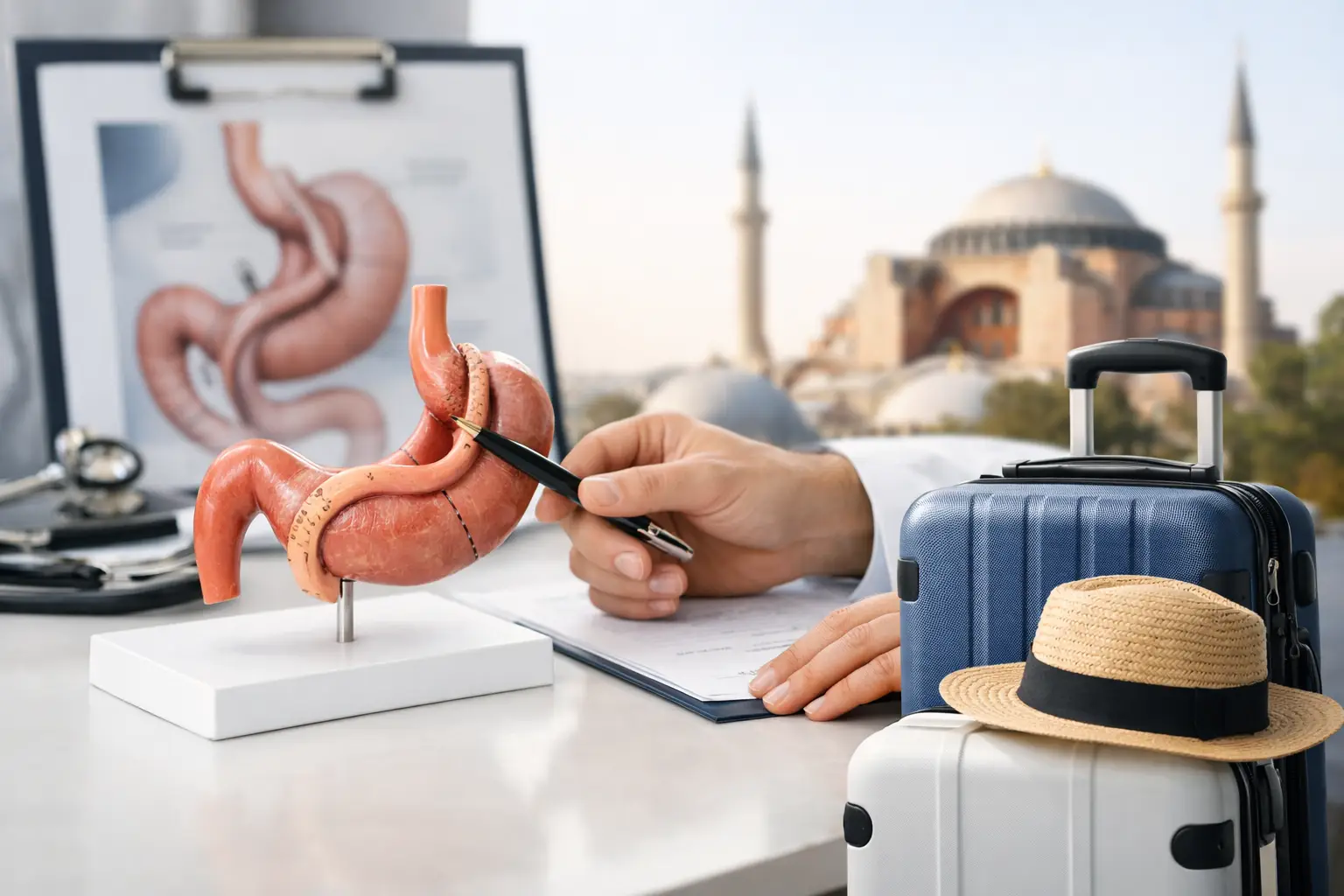
If you are booking bariatric surgery abroad, one detail can change the entire experience: having an English-speaking patient advocate in Turkish hospitals who stays with you through the practical, clinical and emotional parts of the journey. When you are trying to understand consent forms, pre-op instructions, test results and discharge advice in a different country, clear communication is not a luxury. It is part of safe, calm care.
For many patients, the biggest worry is not the operation itself. It is the fear of missing something important. You may be wondering whether you will understand your surgeon properly, whether your partner will be kept informed, or what happens if you feel unwell and cannot explain it confidently. Those concerns are reasonable. A strong patient advocate helps close that gap.
What an English-speaking patient advocate does in Turkish hospitals
A patient advocate is more than a translator standing at the bedside. In a medical travel setting, the role is usually much broader. They help you understand what is happening, when it is happening, and why it matters. That might mean walking you through admission, accompanying you to blood tests and imaging, explaining what the nursing team needs from you, and making sure your questions reach the right clinician.
In bariatric care, timing and clarity matter. You may need to follow fasting instructions, complete ECG and bloodwork, review your medical history, meet the anaesthetist, and prepare for early mobilisation after surgery. If any part of that process feels unclear, anxiety rises quickly. An advocate provides continuity when several teams are involved.
That continuity matters because hospitals are busy. Surgeons, nurses, porters, admissions staff and hotel drivers may all be excellent at their jobs, but patients still need one clear point of contact. The best advocacy support gives you that familiar voice from arrival through discharge and aftercare follow-up.
Why English-speaking patient advocate support in Turkish hospitals matters in bariatric travel
Weight-loss surgery is not a simple tourist purchase. It is major treatment with real preparation, real recovery and long-term lifestyle change. That means support should not stop at translation. It should include reassurance, coordination and careful communication between you, the clinical team and, where relevant, the family member travelling with you.
This is especially valuable if you are coming from the UK or Ireland and want straight answers without guessing your way through unfamiliar systems. In good hospitals, clinical standards may be high, but if communication feels patchy, confidence can still drop. Patients often judge the quality of care not only by the operation, but by how informed and looked after they felt hour by hour.
An advocate helps reduce that sense of being out of your depth. If you wake after surgery feeling uncomfortable, emotional or confused, you need someone who can explain what is normal, what the team is monitoring, and when the surgeon will review you. That does not replace medical care. It supports your understanding of it.
The difference between advocacy and basic translation
This is where many patients need to look more closely. A hospital may say English is spoken, and sometimes that is true at consultant level, but your day-to-day care usually involves several staff members with different levels of spoken English. There is a clear difference between occasional translation and dedicated advocacy.
Basic translation tends to be reactive. You ask a question and someone helps if available. Advocacy is proactive. The patient advocate checks whether you understand the plan, anticipates common concerns, follows your movement through tests and admission, and helps you raise issues before they become stressful.
For example, after a gastric sleeve or bypass, patients often have practical questions that feel small but matter a great deal at the time. Why am I being encouraged to walk so soon? Is this shoulder pain expected? How much should I sip? What happens if I feel sick in the hotel? A patient advocate who understands bariatric recovery can answer appropriately or quickly bring in the right clinician.
That mix of hospitality and clinical awareness is what gives patients confidence. It is not about making things feel luxurious for the sake of it. It is about making sure you never feel left alone with uncertainty.
What good advocacy looks like before surgery
The quality of support often shows itself well before hospital admission. Strong coordination usually starts with gathering your medical history, reviewing eligibility, helping schedule surgery dates and explaining what to bring, what to stop taking and how to prepare.
At this stage, patients often need plain English more than sales language. They want to know how many nights they will stay, whether a companion can be nearby, how the pre-op tests work, and what the first few days after surgery realistically feel like. Honest preparation is reassuring because it sets expectations properly.
Good advocates also know when not to oversimplify. If a surgeon needs further tests, or if your body mass index, reflux history or previous procedures may affect which operation is most suitable, you should hear that clearly. Reassurance only works when it is tied to accuracy.
What to expect during your hospital stay
Once you arrive in hospital, practical support becomes even more important. Admission paperwork, room orientation, pre-operative checks and consent discussions can all happen quickly. If you are nervous, tired from travelling or worried about the operation, your ability to absorb information may dip.
A well-organised patient advocate helps slow things down enough for you to understand them. They can explain the sequence of the day, repeat instructions in plain terms, and keep your companion informed if appropriate. They also help preserve dignity. Many patients feel vulnerable discussing weight, past health struggles or post-op discomfort. Speaking in your own language helps you say what you really mean.
After surgery, advocacy becomes partly observational. Not in a clinical decision-making sense, but in recognising when you are worried, when you need clarification, or when a concern should be escalated quickly to the nursing or surgical team. That can make the difference between feeling panicked and feeling supported.
How to judge whether a provider really offers this support
Not every company uses the same language, and not every hospital-based service works in the same way. Ask who your main contact will be, whether that person is available in hospital as well as by message, and whether they understand bariatric pathways specifically.
You should also ask what happens outside standard office hours. Recovery does not always wait politely for the next morning. If you are uncomfortable in the evening, worried about hydration, or unsure about medication after discharge, responsive support matters.
Look for specifics rather than broad promises. It is reassuring to hear that someone will meet you at the airport, coordinate your tests, accompany you through admission, communicate with your surgeon, and stay in touch after discharge. Those details are more meaningful than generic claims about customer service.
This is where concierge-style coordination can be especially valuable. When travel, hotel arrangements, hospital scheduling and aftercare sit under one organised process, there are fewer gaps for the patient to manage alone. For bariatric travellers, that joined-up approach often feels safer than arranging each piece independently.
Why this matters after you leave the hospital
The patient journey does not end at discharge. In many ways, this is when questions become more personal. You may be back at the hotel thinking about fluid goals, discomfort, walking, medications and the flight home. Later, once you are back in the UK, your focus shifts to protein intake, vitamins, healing and long-term routine.
An advocate who is part of a proper aftercare structure can help bridge that transition. You should know who to contact, what symptoms need urgent review, and what is expected in the first days and weeks. Patients recovering well still need reassurance. Patients having a wobble need quick, calm guidance.
That is one reason many international patients prefer a managed pathway instead of handling surgery abroad alone. With the right support, the experience feels less like travelling into the unknown and more like moving through a clear plan with people who already know the usual questions and concerns.
For anyone considering weight-loss surgery abroad, the value of an English-speaking patient advocate in Turkish hospitals is simple. It turns confusing moments into clear ones and stressful moments into manageable ones. And when you are making a serious decision about your health, that kind of support is never a small extra. It is part of feeling safe enough to move forward.