You can usually tell which operation someone wants within the first five minutes of a call. If reflux has been making nights miserable, they lean one way. If diabetes has been a long, exhausting battle, they lean another. And if they have tried every diet under the sun, they often just want the option that feels simplest.
When you are considering bariatric surgery abroad, the decision becomes even more personal. You are not only choosing a procedure – you are choosing how you will live day to day afterwards, how your body will cope with vitamins, and how your health conditions are likely to respond. This is exactly why “gastric sleeve vs gastric bypass Turkey” is not really a debate. It is a matching exercise.
Gastric sleeve vs gastric bypass Turkey: the real difference
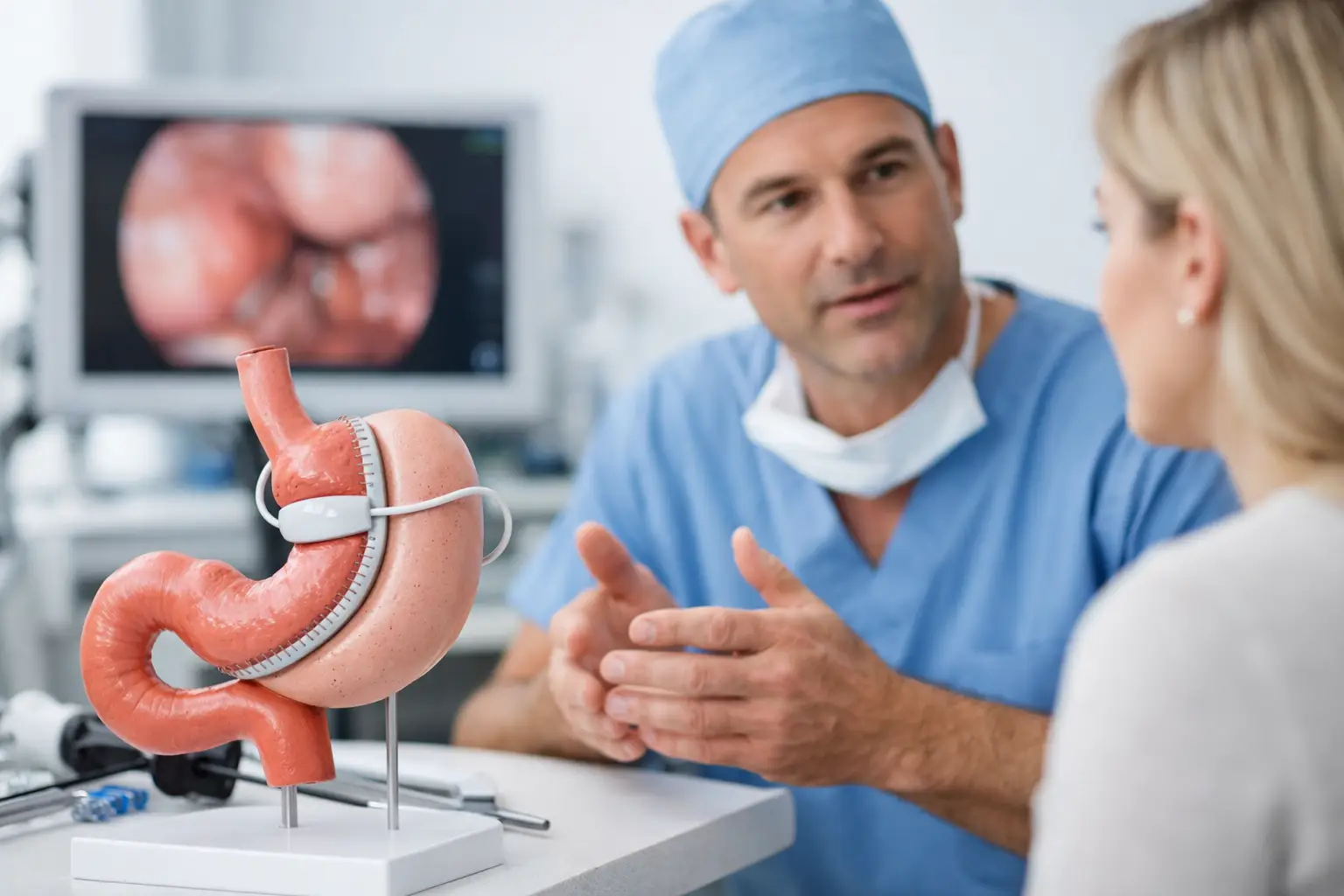
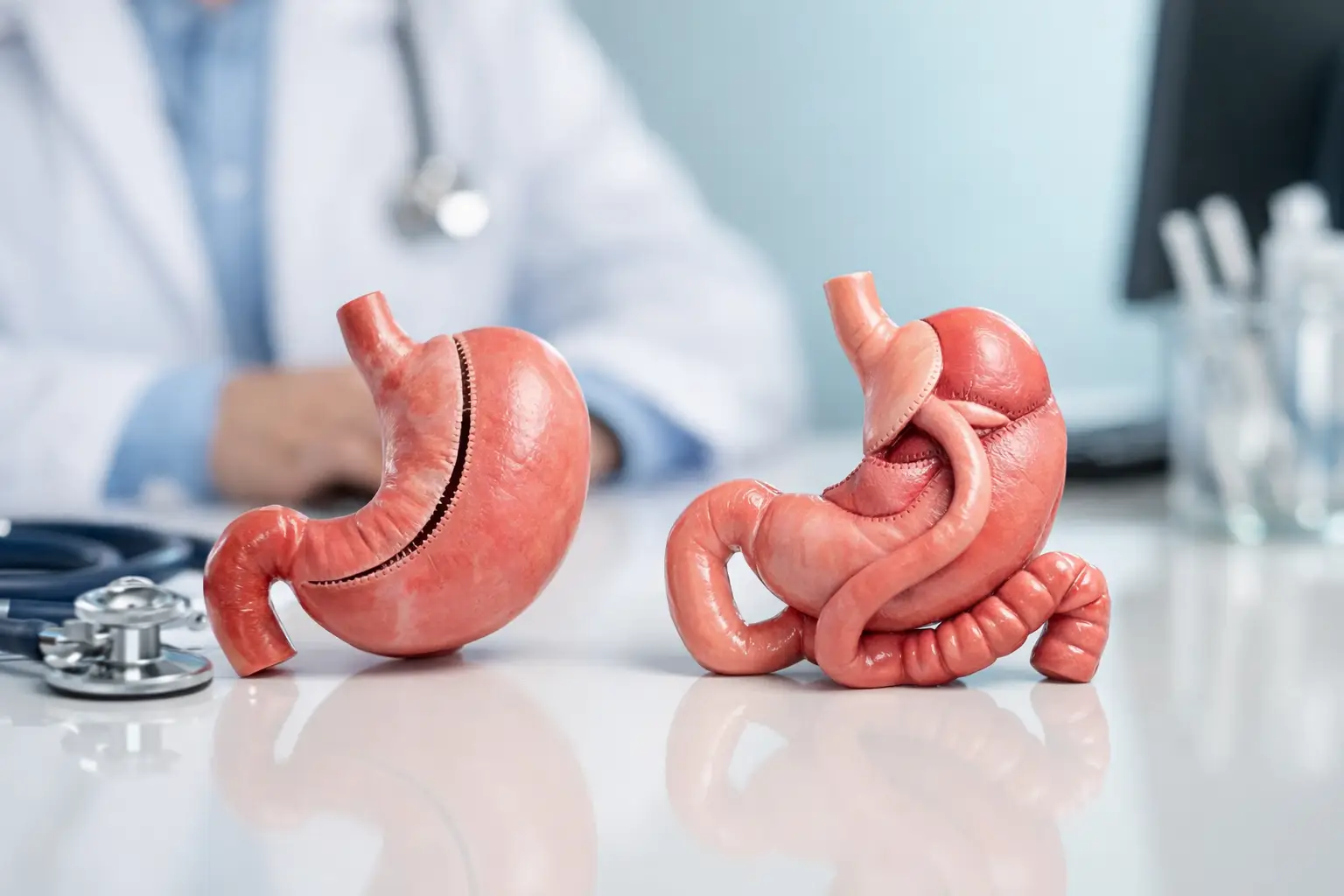
A gastric sleeve (sleeve gastrectomy) reduces the stomach into a narrow “sleeve”. You feel full sooner and, for many people, appetite hormones drop noticeably. There is no rerouting of the bowel.
A gastric bypass creates a small stomach pouch and reroutes part of the small intestine. You eat less, but you also absorb fewer calories and nutrients. Hormonal changes are often stronger, which is why bypass is widely respected for metabolic conditions such as type 2 diabetes.
Both are established, well-studied procedures. Both can be life-changing. The better question is which one fits your medical profile, your lifestyle, and the risks you can comfortably manage.
How weight loss tends to compare
In practical terms, both sleeve and bypass can produce significant, durable weight loss when paired with proper follow-up and a realistic approach to food.
Bypass often has the edge for higher starting BMIs and for patients who have struggled to maintain loss after many attempts. The malabsorption component and hormonal impact can make weight loss more consistent for some people.
Sleeve outcomes can be excellent, particularly for patients without severe reflux and with a strong commitment to structured eating. Many patients like that it is anatomically simpler and does not involve intestinal rerouting.
What matters most is less about “which one loses more” and more about what helps you keep it off. That comes down to satiety, food tolerance, follow-up, and whether there are medical issues that push you towards one procedure.
Reflux: the make-or-break factor for many patients
Reflux is where the decision often becomes clear.
Sleeve can worsen reflux in some patients, particularly if reflux is already present or if there is a hiatal hernia that needs addressing. Some people do very well after sleeve, but if your heartburn is frequent, your surgeon may advise bypass instead.
Bypass is commonly recommended for patients with significant gastro-oesophageal reflux disease because it tends to improve symptoms. If you are already sleeping propped up on pillows, taking regular acid suppression, or avoiding foods because of burning pain, bring this up early. It is not a small detail – it can be the deciding factor.
Type 2 diabetes and metabolic conditions
If your priority is metabolic improvement, bypass is often the stronger tool.
Many patients see rapid improvements in blood sugar control after bypass, sometimes within days, because of powerful hormonal changes. Sleeve can also improve diabetes, particularly when the condition is earlier and weight-driven, but bypass has a longer track record for remission rates in appropriate patients.
If you are on insulin, have had diabetes for many years, or have other metabolic complications, your surgical team will consider bypass more seriously. It is not about chasing the “most dramatic” option – it is about choosing the operation most likely to change your health trajectory.
Vitamins, supplements, and long-term maintenance
This is the part many people underestimate, and it matters for life.
After sleeve, you still need vitamins, but absorption is largely preserved. Patients typically take a bariatric multivitamin and may need extra iron, vitamin D, or B12 depending on blood results.
After bypass, vitamin and mineral supplementation is non-negotiable. Because absorption is reduced, long-term deficiencies are more likely without consistent supplements and periodic blood tests. Most patients do very well with a clear plan, but it does require commitment. If you travel frequently, have a history of anaemia, or struggle with taking tablets, it is worth discussing openly.
A good team will not shame you for this – they will help you plan for reality.
Food tolerance and day-to-day life afterwards
Both surgeries change how you eat. The first months are structured: liquids, then purees, then soft foods, then gradual progression.
With sleeve, patients often report strong restriction and early satiety. Some find they can eat a wider variety of foods later on, but portions remain small.
With bypass, some people are more sensitive to sugar and high-fat foods. “Dumping” symptoms can happen – sweating, nausea, cramping, light-headedness – especially after sugary foods. Many patients see this as helpful guardrails; others find it unpleasant. Not everyone experiences dumping, but the risk is part of the bypass trade-off.
If you have a sweet tooth and want a procedure that makes sugary foods less appealing, bypass can support that. If you prefer fewer “built-in consequences” and have no reflux, sleeve may feel more straightforward.
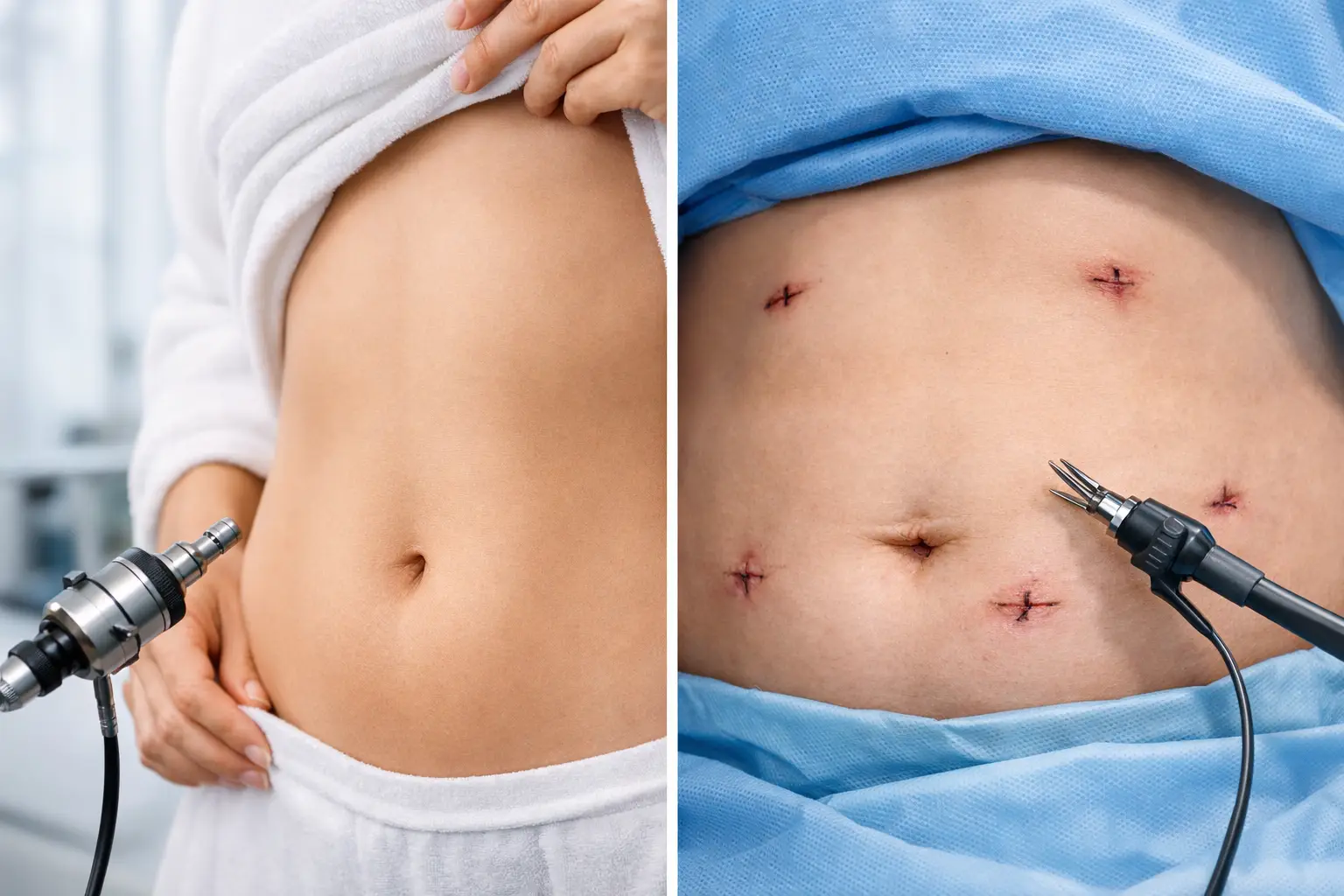
Safety and surgical complexity
Both operations are major surgery. In skilled hands and with proper screening, complication rates are low, but no responsible provider will describe either as risk-free.
Sleeve is generally a shorter operation and is often described as less complex anatomically. The main concerns include staple-line leaks, bleeding, and reflux issues.
Bypass is more complex, with additional connections (anastomoses). Risks can include leaks, internal hernias, and strictures, alongside nutritional deficiencies long term.
When patients ask, “Which is safer?” the honest answer is that safety is not only about the name of the procedure. It is about patient selection, surgeon experience, hospital standards, pre-op testing, and post-op support.
Why Turkey, and why logistics matter more than you think
Many UK patients choose Turkey because it can offer faster scheduling and better value than private options at home, without compromising on modern hospitals and experienced bariatric teams. Antalya, in particular, is a place where medical care and hospitality infrastructure naturally go together.
But the outcome is not only about the operation. It is also about how smoothly your days around surgery are managed: airport pick-up when you are tired and anxious, hotel check-in, translation when you are asked clinical questions, and organised pre-op tests so you are not running around a city you do not know.
This is where a coordinator-led approach reduces stress and prevents missed steps. If you are exploring options, Bridge Health Travel works as a concierge-style partner in Antalya, aligning surgery planning with transfers, accommodation, pre-op tests, and structured aftercare check-ins once you are back in the UK.
Who is often better suited to sleeve?
Sleeve can be a strong fit if you do not have significant reflux, you want an operation without intestinal rerouting, and you are comfortable with the idea that weight maintenance will rely heavily on portion control, protein-first eating, and routine.
It can also suit patients who want an effective primary procedure and may consider a revision later if needed. That is not a “failure plan”. It is simply acknowledging that obesity is a chronic condition and treatment can be staged.
Who is often better suited to bypass?
Bypass is often favoured when reflux is a major issue, when diabetes control is a central goal, or when the starting BMI and metabolic risk suggest you need the stronger metabolic push.
It can also be appropriate for patients who have had a sleeve before and are dealing with weight regain or reflux afterwards. Revisional surgery is highly individual, and imaging plus surgeon review are essential, but bypass is commonly part of the discussion.
Questions to ask before you choose
A good decision usually comes from a short set of very direct questions. Ask what your reflux risk is with sleeve, and whether a hiatal hernia is present. Ask what your vitamin plan will look like at 6 months, 12 months, and beyond, and how often you should test your bloods once you are home. Ask what your realistic weight-loss range is for your BMI and health conditions, not someone else’s.
Also ask about aftercare contact. The weeks after surgery can feel emotionally strange: you may be thrilled, then suddenly tearful, then worried you are not losing “fast enough”. A team that stays present after you fly home can make the difference between panic-Googling symptoms at midnight and getting calm, clinically sound guidance.
A closing thought
Try not to pick your surgery based on the one that sounds more powerful, or the one a friend had. Choose the one that matches your body’s realities – reflux, diabetes, eating patterns, supplement commitment – and then build your success around steady follow-up and patient, consistent habits. That is where the confidence comes from, long after the flight home.