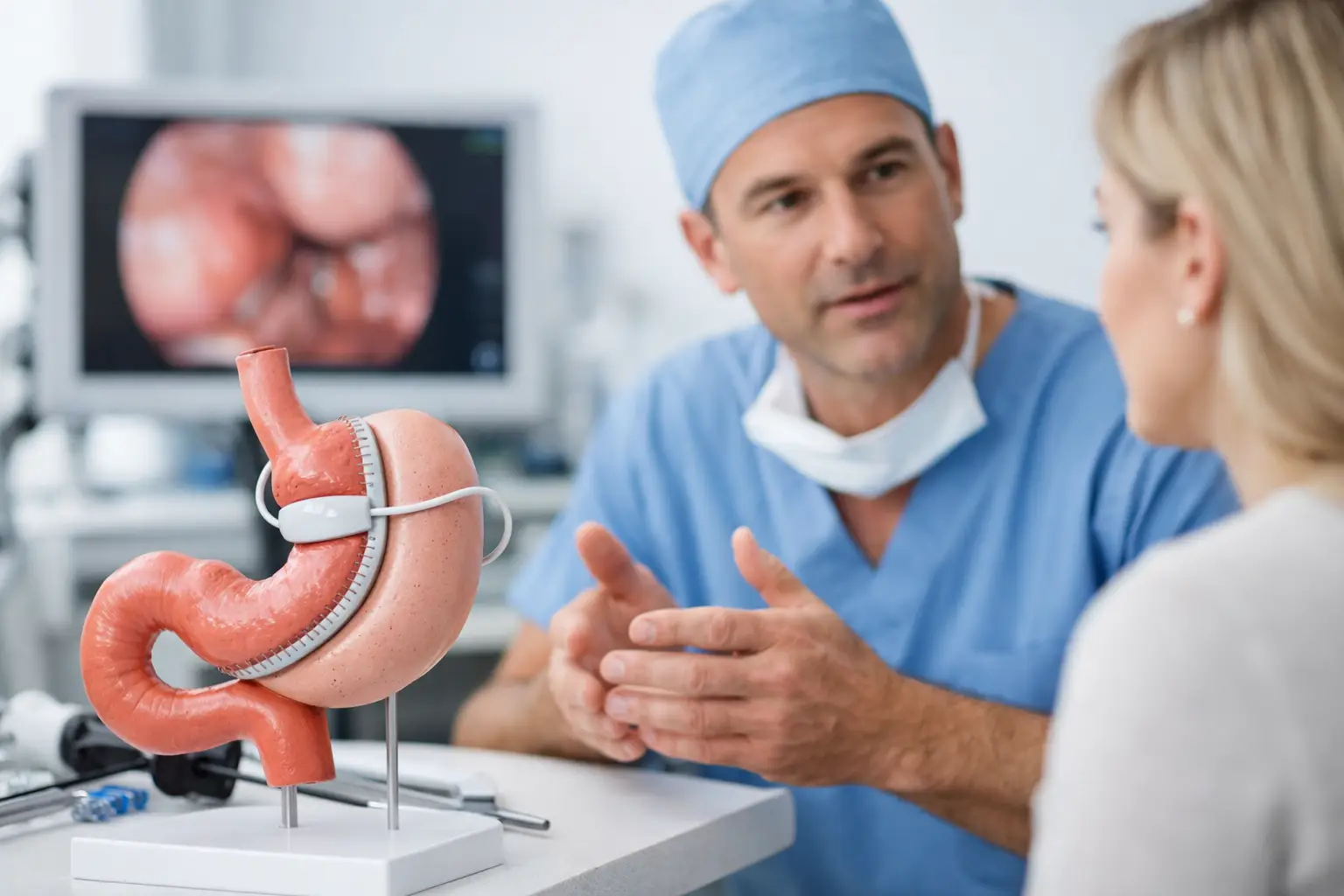
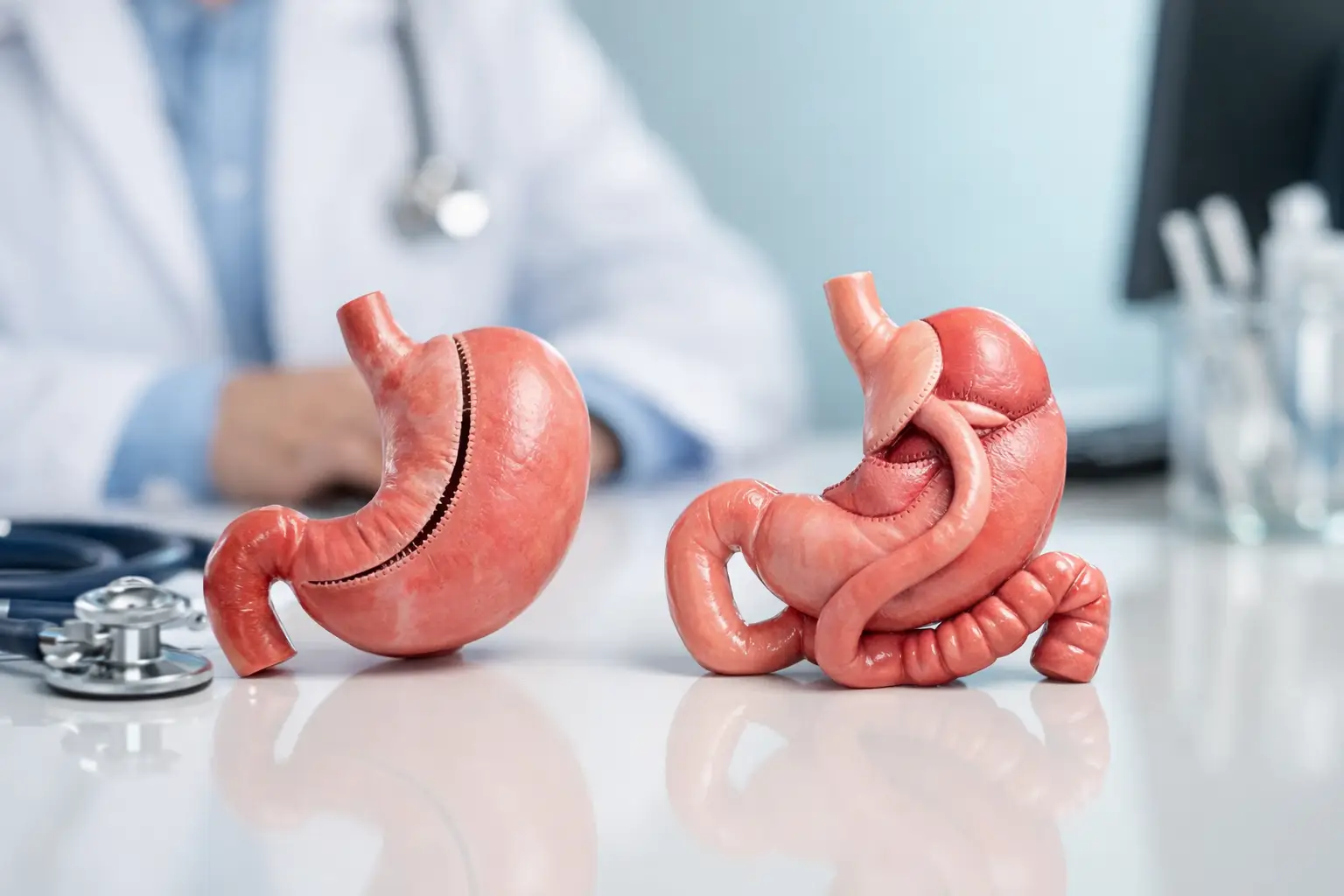
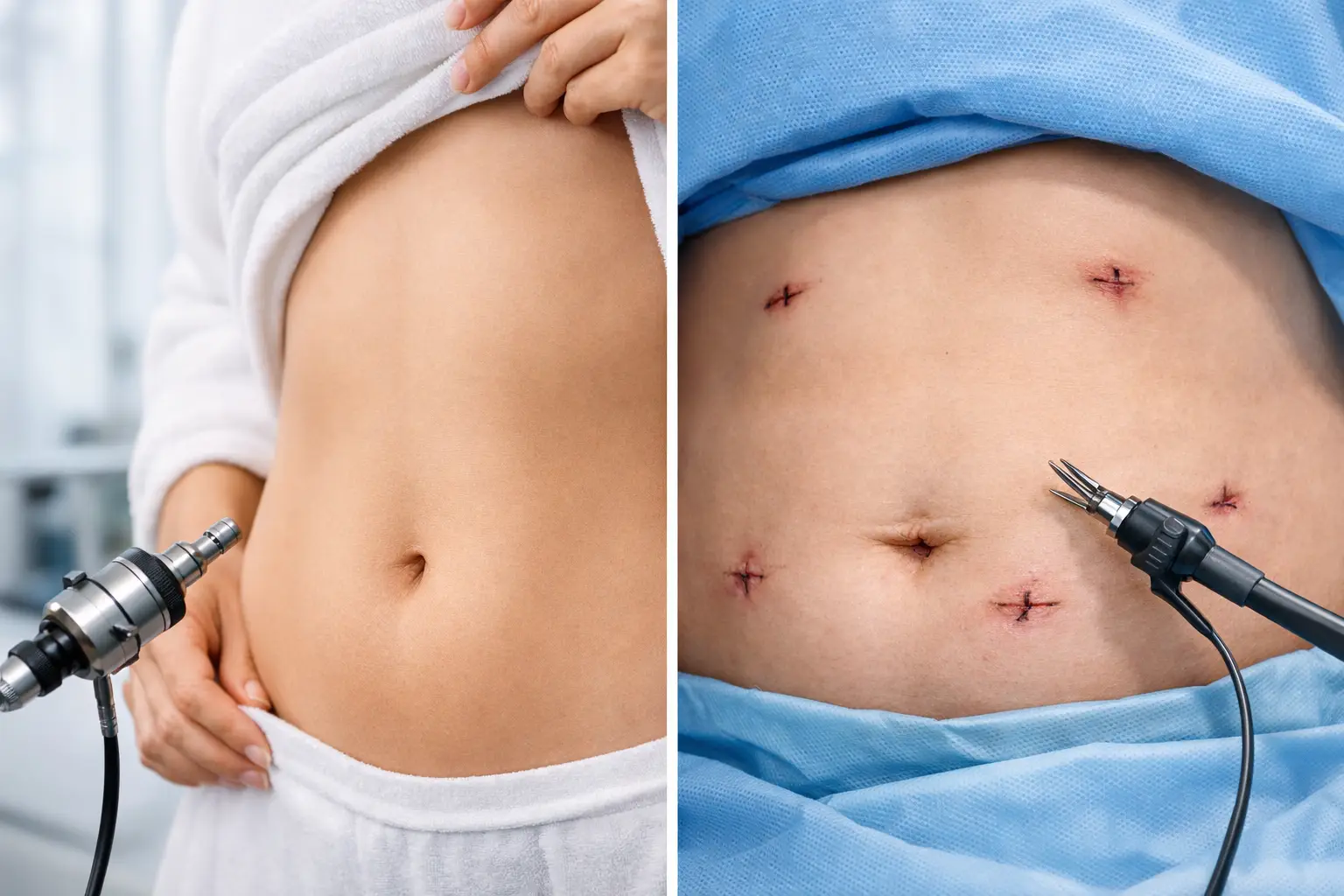
A year or two after weight-loss surgery, the questions can feel surprisingly quiet at first. You notice your portions creeping up, the scales stalling, reflux that never quite settles, or a sense that your first operation simply did not give you the tool you were promised. If you are now searching for revisional bariatric surgery in Turkey, you are usually not looking for “more willpower”. You are looking for a clear explanation of what changed, what can be corrected, and how to do it safely.
What revisional bariatric surgery actually means
Revisional bariatric surgery is not a cosmetic tweak and it is not a sign of failure. It is a planned second operation (or occasionally a corrective procedure) to address problems after a primary bariatric surgery. Those problems tend to fall into three buckets: inadequate weight loss or significant regain, complications that affect quality of life (such as reflux), or a technical issue with the original anatomy (such as dilatation of the sleeve or pouch).
A revision can be “conversion” surgery (changing one operation to another), “re-do” surgery (refashioning the existing procedure), or a corrective fix to deal with a complication. The right approach depends on what is happening inside your stomach and small bowel now, not what the operation was meant to do on paper.
Why people consider revisional bariatric surgery Turkey
For UK patients, the decision often starts with timing and access. Revisions can involve long waits, strict criteria, or limited local availability – even when symptoms are affecting daily life. Turkey, and Antalya in particular, has become a practical option because patients can be assessed quickly, operated on in hospital settings that run bariatric pathways every day, and supported with structured logistics.
Cost matters too, but most people do not choose revision purely on price. Revision is higher-stakes than a first operation. Patients who travel want a team that can run proper pre-op checks, coordinate imaging and bloods promptly, and manage the early post-op phase closely – especially if you are flying home within days.
When revision is worth discussing (and when it may not be)
If you have had weight regain, it is tempting to assume the anatomy has “stretched” and a revision is the answer. Sometimes it is. But it depends.
If regain is mainly behavioural (grazing, liquid calories, alcohol, poor protein routine), revision may give only a short-lived effect unless the day-to-day structure changes as well. A reputable team will talk to you about this plainly and may ask for a diet history, symptoms timeline, and weight curve before suggesting surgery.
On the other hand, certain patterns are strong signals that a surgical solution might be appropriate. Severe reflux after sleeve gastrectomy, vomiting or food intolerance due to a narrowing, persistent pain, ulcers, or confirmed dilatation of the sleeve/pouch can make revision less about weight and more about restoring quality of life and safety.
Common revision pathways (and why one might suit you)
There is no single “best” revisional operation. The best option is the one that matches your current anatomy, symptoms, and health profile.
Sleeve to gastric bypass (often for reflux)
If you have a gastric sleeve and struggle with ongoing reflux that does not respond to medication, conversion to a Roux-en-Y gastric bypass is a well-established option. For many patients, it reduces acid exposure because the new anatomy diverts bile and acid away from the oesophagus. It can also support further weight loss if regain has occurred.
Trade-off: bypass brings a stronger malabsorptive component than sleeve. That means lifelong vitamins are non-negotiable, and follow-up blood tests matter.
Sleeve to mini gastric bypass (one-anastomosis)
Some patients are offered a mini gastric bypass as a conversion option, particularly when the aim is further weight loss and appetite control. It uses a single join to the small bowel and can be an efficient revision in experienced hands.
Trade-off: mini bypass can be associated with bile reflux in a subset of patients. A good consultation will explore your reflux history carefully and discuss which bypass configuration best fits your symptoms.
Re-sleeve or sleeve tightening (selected cases)
If imaging shows the sleeve has dilated significantly and reflux is not the main problem, a re-sleeve may be considered. This is not appropriate for everyone, and it is not the first choice when reflux is present.
Trade-off: because it is working on scar tissue, re-sleeve can carry higher leak risk than a primary sleeve. Surgeon experience and hospital protocols become even more important.
Band removal and conversion
If you previously had a gastric band and have regain, reflux, intolerance, or slippage, band removal with conversion to sleeve or bypass is common. The best choice depends on your oesophageal motility, reflux, and scarring.
Trade-off: sometimes removal and conversion are best done as a staged approach for safety, particularly if there is inflammation.
Safety first: what good revision planning looks like
Revisional bariatric surgery should feel more investigative than a first-time pathway. You are not just picking a procedure; you are confirming what is happening now.
A thorough plan typically includes bloodwork (including iron studies, B12, folate, vitamin D and metabolic markers), ECG, and imaging tailored to your symptoms. Many patients benefit from an upper GI contrast study or endoscopy to assess sleeve shape, pouch size, narrowing, ulcers, hiatal hernia, or gastritis. If reflux is part of your story, it is also important to evaluate for a hiatal hernia and discuss whether hernia repair is needed alongside the revision.
Just as important is an honest review of your medical risks: smoking status, diabetes control, sleep apnoea, blood pressure, clotting risk, and previous abdominal surgery. Revision should not be rushed, but it can still be efficient when the pathway is organised properly.
What your Antalya experience should feel like (logistics and care)
If you are travelling for surgery, your stress levels often have less to do with the flight and more to do with uncertainty: Who meets you? Where do you go? What happens if you feel unwell at 2am? Revision patients need calm, not guesswork.
In a well-run Antalya pathway, the journey is tightly scheduled. You should expect airport pick-up, hotel arrangements that fit your pre-op fasting and rest needs, and a clear plan for pre-operative tests. In hospital, revision patients benefit from private rooms, frequent nursing checks, early mobilisation support, and daily surgeon review – because small issues (nausea control, hydration, pain) are best handled early.
This is exactly where a coordinator-led service can make a practical difference. With Bridge Health Travel, for example, patients are guided from planning to transfers, tests, hospital scheduling, translation support, and structured aftercare check-ins once they return home.
Recovery and aftercare: what changes after a revision
Most patients are surprised by two things after revision. First, the first week can feel more intense than their original surgery, especially if adhesions were present or the operation was complex. Second, the long-term success relies even more heavily on routine.
You will usually start with a staged diet progression, strict hydration targets, and a focus on protein as soon as permitted. If your revision involves bypass, vitamin and mineral supplementation is lifelong. If your revision was prompted by reflux, you will want clear guidance on medication timing, trigger foods, and when symptoms should be improving.
It is also wise to plan your return flight with realistic comfort in mind. Compression stockings, walking during the journey when safe, and your team’s advice on clot prevention are not optional extras. If you have a history of clots or significant risk factors, your surgeon may recommend injectable anticoagulation for a period.
Choosing the right team for revisional bariatric surgery in Turkey
Revision is not the time to shop by headline price or social media photos. You want to know how decisions are made.
Ask direct questions: What is the suspected cause of my symptoms or regain? What tests will confirm it? Which revision do you recommend and why not the alternatives? How do you manage leaks, strictures, bleeding, and reflux if they occur? How often does this surgeon perform revisions like mine?
You should also look for clarity around follow-up. A revision patient needs responsive communication after discharge, because dehydration, nausea, constipation, or anxiety can escalate quickly if you feel alone. A good programme will check in, adjust medications, and advise when you should seek in-person assessment at home.
The most reassuring sign: a plan that fits you
The best outcome is not “the biggest operation”. It is the operation that matches your anatomy, symptoms, and lifestyle – with enough support to help you keep the result.
If you are considering revisional bariatric surgery Turkey, give yourself permission to treat it like a careful reset, not a desperate last step. The right team will be calm, specific, and evidence-led, and you should feel that your questions are welcome right up to the moment you fly home – and long after you unpack.