You have the flight in mind, you have the procedure in mind, and then the nerves arrive: “What if I turn up in Turkey and they tell me I can’t have surgery?” Pre-op testing is designed to prevent that moment. It is not a box-ticking exercise. These checks confirm you are fit for anaesthetic, help the surgeon choose the safest approach, and reduce the risk of surprises once you are on the ward.
When patients ask about bariatric surgery pre op tests Turkey hospitals require, what they usually want is clarity: which tests, when they happen, what might delay surgery, and how the results affect the plan. The reassuring part is that the process is structured and predictable, and good clinics build time into your schedule to complete it properly.
What “pre-op tests” really do
Pre-operative tests have three jobs. First, they identify medical risks that could make anaesthesia unsafe right now, such as uncontrolled blood pressure, an active infection, or significant heart rhythm issues. Second, they map out practical details for surgery – for example, whether you are anaemic, whether your liver enzymes are elevated, or whether your blood sugar control needs tightening. Third, they allow the team to tailor your care, from blood clot prevention to pain relief choices.
There is a trade-off here. A thorough pre-op work-up can feel intense, especially if you have had years of “normal” GP appointments. But bariatric surgery is a major intervention, and being precise before you go to theatre is one of the reasons outcomes are so strong when patients are properly screened.
When and where testing happens in Turkey
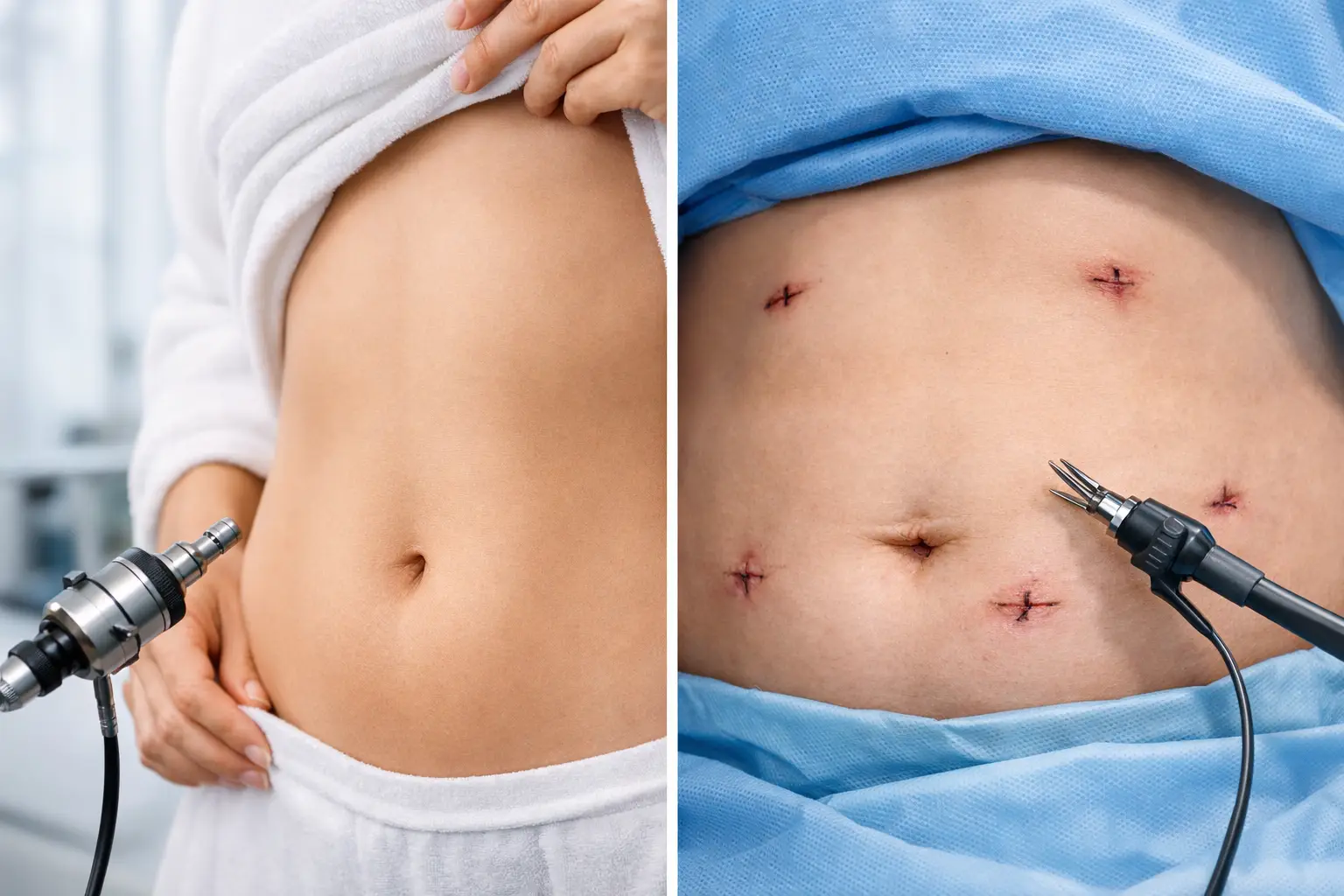
Most international patients do their main testing after arrival, typically on the day of admission or the day before surgery depending on the hospital pathway. This is common in medical travel because it ensures results are recent and captured in the hospital’s own systems.
That said, if you have complex health conditions or a history that raises questions – previous clots, significant heart disease, lung disease, or multiple prior abdominal operations – you may be asked to supply recent reports before you travel. It depends on your clinical history and how much certainty the surgeon needs in advance.
If you work with a facilitator that coordinates care end-to-end, your schedule is usually designed so testing, consultant review, and surgical sign-off happen in a logical order. With Bridge Health Travel, this coordination is built into the patient journey, so you are not trying to interpret results or chase departments while you are also adjusting to a new country.
The core bariatric surgery pre op tests Turkey clinics commonly request
Blood tests (bloodwork)
Bloodwork is the backbone of pre-op screening. It helps the team spot hidden issues that can increase surgical risk or slow healing.
Most patients can expect a full blood count (to check for anaemia or infection markers), kidney function and electrolytes (important for safe fluid balance during and after surgery), liver function tests, clotting profile, and blood glucose markers. Many teams also check iron stores, vitamin B12, folate, vitamin D, and sometimes thyroid function, because bariatric patients can arrive with deficiencies that matter after surgery.
Abnormal results do not automatically mean “no surgery”. Mild deficiencies are often treated with supplements and a plan for post-op monitoring. More significant issues may mean postponing until corrected – frustrating, but far safer than rushing into theatre with avoidable risk.
ECG (heart tracing)
An ECG is quick but valuable. It looks for rhythm problems, past silent heart events, or conduction changes that might affect anaesthetic management. If your ECG is abnormal or you have cardiac symptoms, the anaesthetist may request further assessment. That could be as simple as a repeat ECG and a clinical review, or it could involve an echocardiogram.
This is one of the places where honesty in your medical history matters. If you have chest pain on exertion, unexplained breathlessness, or a strong cardiac history, say so early. It allows the team to plan properly rather than scrambling on admission day.
Chest imaging (often a chest X-ray)
Chest imaging helps rule out active lung issues and gives the anaesthetist information relevant to airway and ventilation planning. For smokers, those with asthma or COPD, or patients with frequent chest infections, this can be particularly informative.
If you have symptoms of a current infection, surgery may be delayed until you are well. Anaesthesia plus a respiratory infection is an avoidable risk, and postponing by a short period can prevent a longer, more difficult recovery.
Abdominal ultrasound
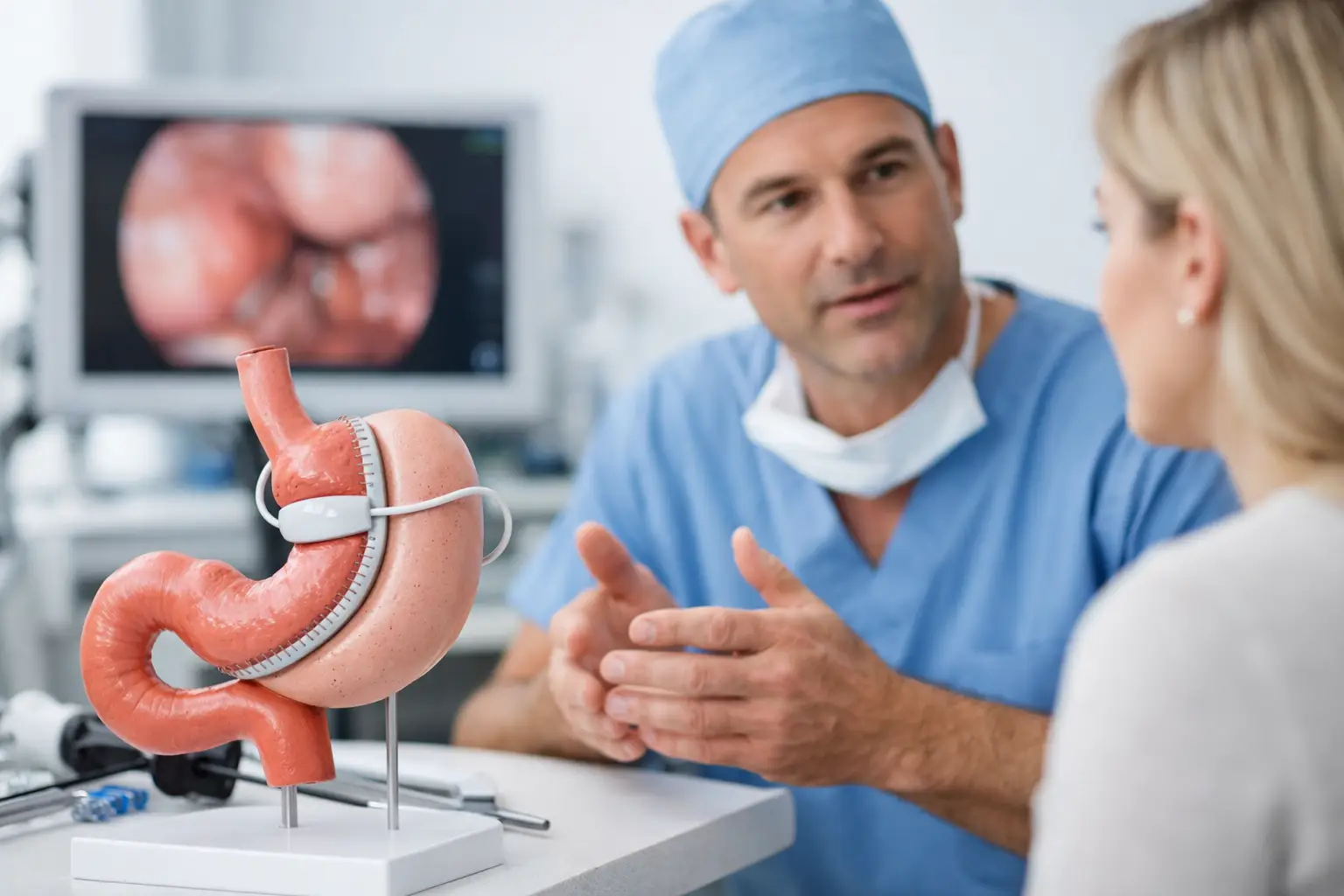
Many bariatric pathways include an abdominal ultrasound to check the liver and gallbladder. A fatty liver is common in obesity and can affect surgical access, particularly in gastric sleeve surgery where the surgeon needs safe visibility at the top of the stomach.
Gallstones are another common finding. Sometimes this simply means you will be counselled about symptoms and future management. In selected cases, it may influence the surgical plan. It depends on severity, symptoms, and the surgeon’s approach.
Endoscopy (only for some patients)
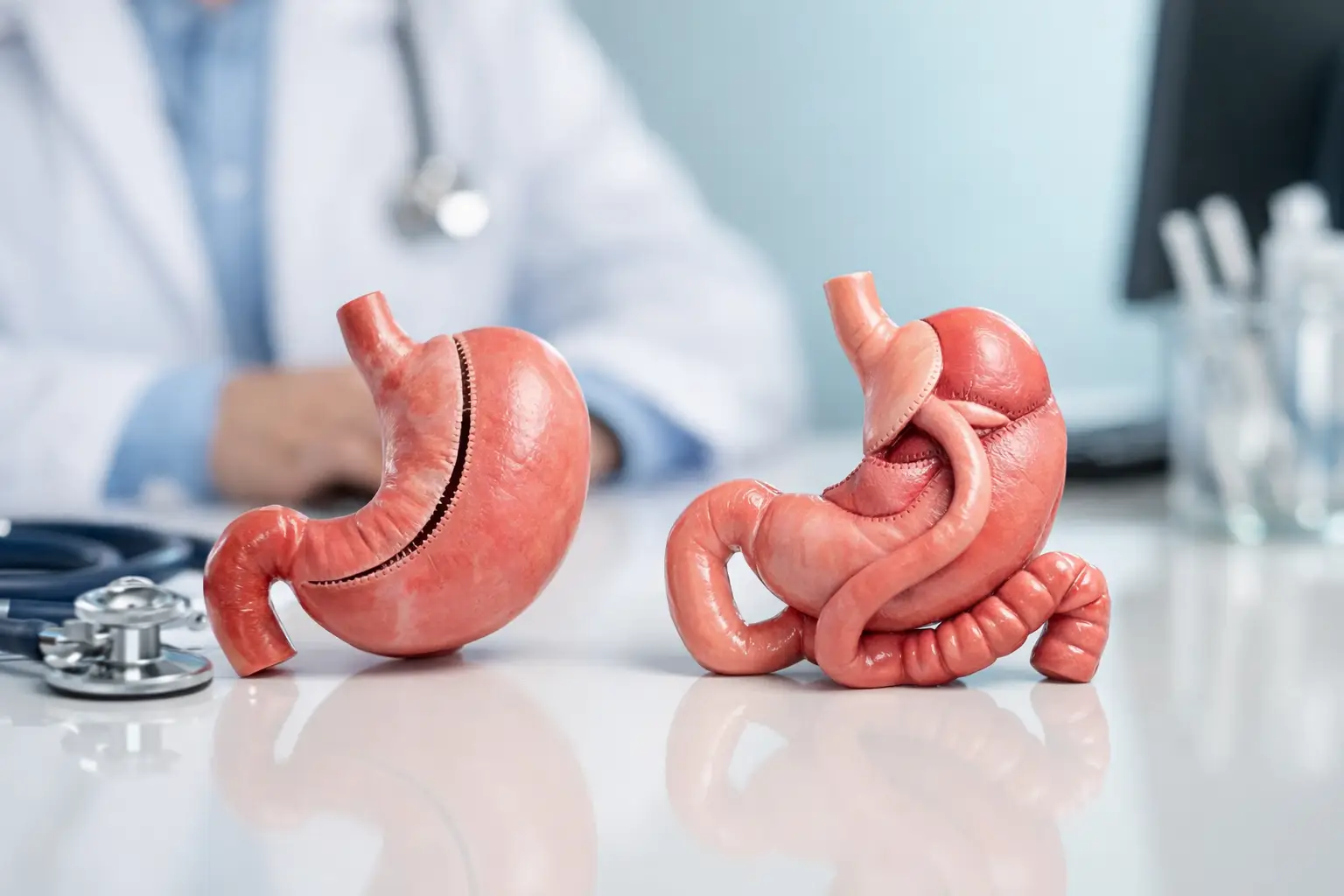
Not every patient needs an endoscopy, but it may be recommended if you have reflux symptoms, a history of ulcers, long-term acid suppression medication, or concerns about a hiatal hernia. It can change the best procedure choice – for example, significant reflux can steer some patients away from a sleeve and towards a bypass-style procedure.
This is a good example of tests protecting your long-term outcome, not just getting you through surgery day.
Sleep apnoea screening and respiratory assessment
Many bariatric patients have obstructive sleep apnoea, diagnosed or not. If you already use CPAP, bring that information and your settings. If you have loud snoring, daytime sleepiness, or witnessed apnoeas, tell your coordinator and surgeon.
In some cases, additional screening is arranged. Sleep apnoea affects anaesthetic risk and post-op monitoring needs. Planning for it is straightforward – ignoring it is not.
How results can change your surgery plan
Pre-op tests are not separate from the procedure decision. They are part of choosing the right operation for your body and your long-term health.
If testing shows uncontrolled diabetes or very high blood pressure, the team may stabilise you first. If reflux appears significant, the conversation may shift towards bypass options. If the liver looks very enlarged, you may be asked to follow a strict pre-op diet for a little longer to reduce liver volume and improve surgical access. These adjustments are not setbacks. They are what a safety-first programme looks like.
What to bring from the UK
You do not need to arrive with a suitcase full of paperwork, but a few items can prevent delays.
Bring a list of your current medications with doses, any recent clinic letters (especially cardiology, respiratory, or endocrine), and details of allergies or past reactions to anaesthesia. If you have had previous abdominal surgery, any operation notes can be helpful, but it is not always essential.
If you have recent blood tests from your GP or a private provider, they can provide context, even if the hospital repeats testing on arrival.
Common reasons surgery is delayed after testing
Delays are not common when patients are well-prepared, but they can happen. The most frequent reasons are signs of infection, poorly controlled blood pressure, unstable blood sugars, significant anaemia, or unexpected cardiac or respiratory findings.
If a delay happens, ask the team to explain the exact issue and what would make it safe to proceed. A good provider will give you a clear, practical plan rather than vague reassurance.
How to reduce anxiety before test day
The waiting is often harder than the tests. Two things usually help most. First, understand that many “abnormal” results are manageable and do not end the journey – they simply guide safer care. Second, keep your pre-op diet and hydration instructions exactly as given. Patients sometimes focus on the medical tests and overlook the basics, but following the plan can materially improve results, especially liver size and blood sugar stability.
If you are travelling with a partner or family member, involve them. Having someone else hear the explanations, timings, and next steps can make the day feel calmer and less rushed.
A final thought before you travel
Pre-op tests can feel like the last obstacle between you and a new start, but they are really the first act of good aftercare. When your results are reviewed carefully and your plan is personalised, you are not just getting surgery in Turkey – you are getting a safer operation and a smoother recovery, with fewer “what ifs” left hanging in the air.