Reflux can turn a weight-loss decision into a more complicated conversation. If you are researching the best bariatric surgery for reflux, the right answer is often not the most popular operation overall, but the one that fits your symptoms, scan results, eating pattern and long-term goals.
For many patients, this is the point where things feel confusing. A procedure that works very well for weight loss may not be the best choice if you already have frequent heartburn, regurgitation, a diagnosed hiatus hernia or reflux that needs daily medication. That is why reflux should never be treated as a side note in your bariatric assessment.
Which is the best bariatric surgery for reflux?
In most cases, Roux-en-Y gastric bypass is considered the best bariatric surgery for reflux. It tends to reduce acid exposure and improve symptoms more reliably than sleeve gastrectomy. That matters because the sleeve can worsen reflux in some patients, even when weight loss itself is successful.
That said, there is no one-size-fits-all answer. Some patients have mild, occasional reflux and are still suitable for a sleeve. Others have severe gastro-oesophageal reflux disease, inflammation seen on endoscopy, or a large hiatus hernia, and they are usually better served by a bypass or by a revisional procedure if they have already had a sleeve.
The key point is simple: if reflux is part of your history, procedure choice needs to be led by anatomy and symptoms, not by trend.
Why reflux matters before bariatric surgery
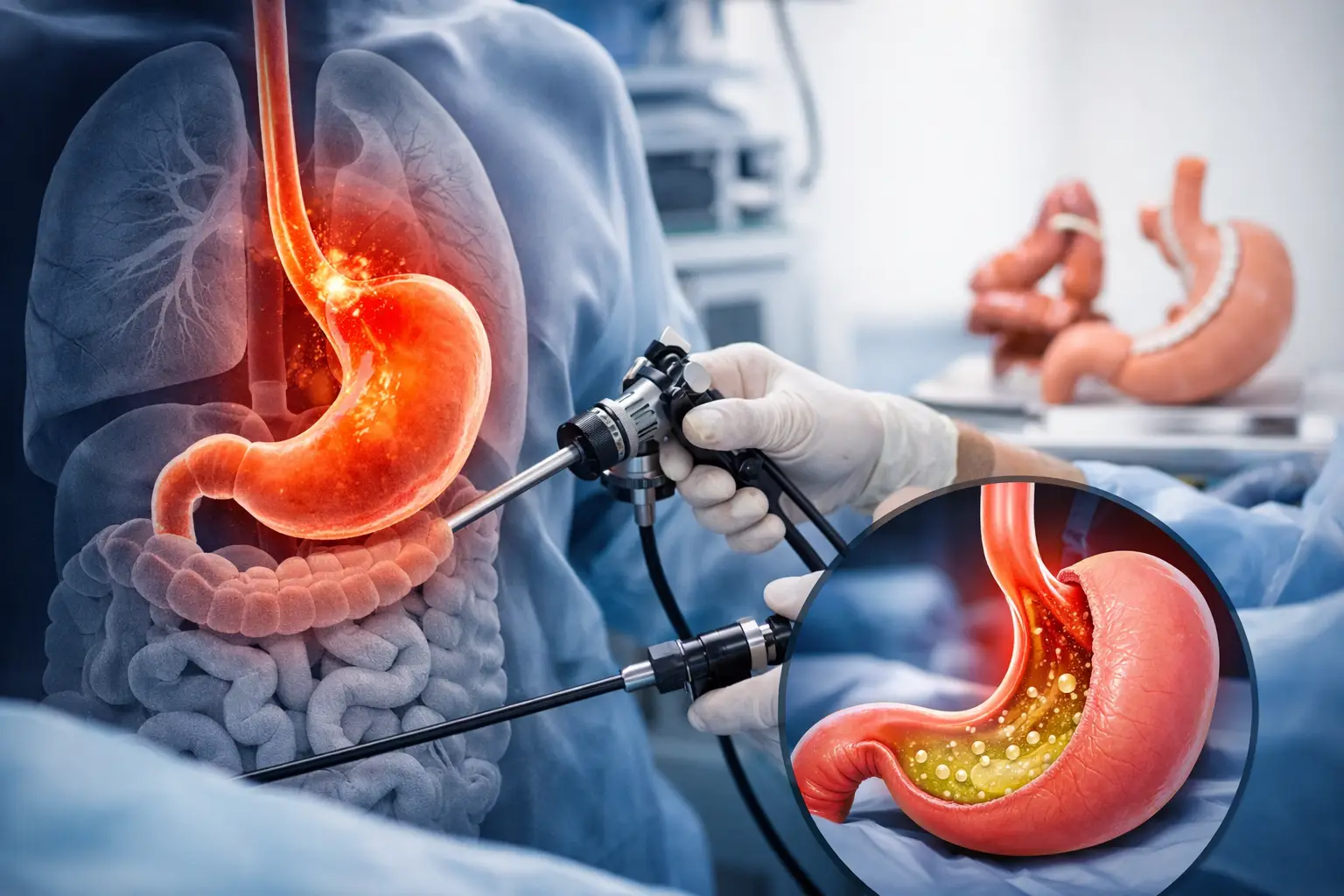
Heartburn after a heavy meal is one thing. Ongoing reflux is different. Chronic acid exposure can affect sleep, quality of life and the oesophagus itself. Some patients describe a burning chest, sour fluid coming up into the throat, coughing at night or needing to sleep propped upright. These details matter because they help your surgical team understand how active the problem is.
Obesity and reflux are closely linked. Extra abdominal pressure can push stomach contents upwards, and a hiatus hernia can make that worse. Weight loss often improves reflux overall, but the type of bariatric operation still matters because each procedure changes the stomach in a different way.
A careful pre-operative work-up usually includes symptom review, medication history, and often endoscopy or imaging when indicated. This is one of the reasons a structured, coordinator-led pathway helps. When testing, surgeon review and travel plans are properly organised, patients feel less like they are piecing together medical decisions on their own.
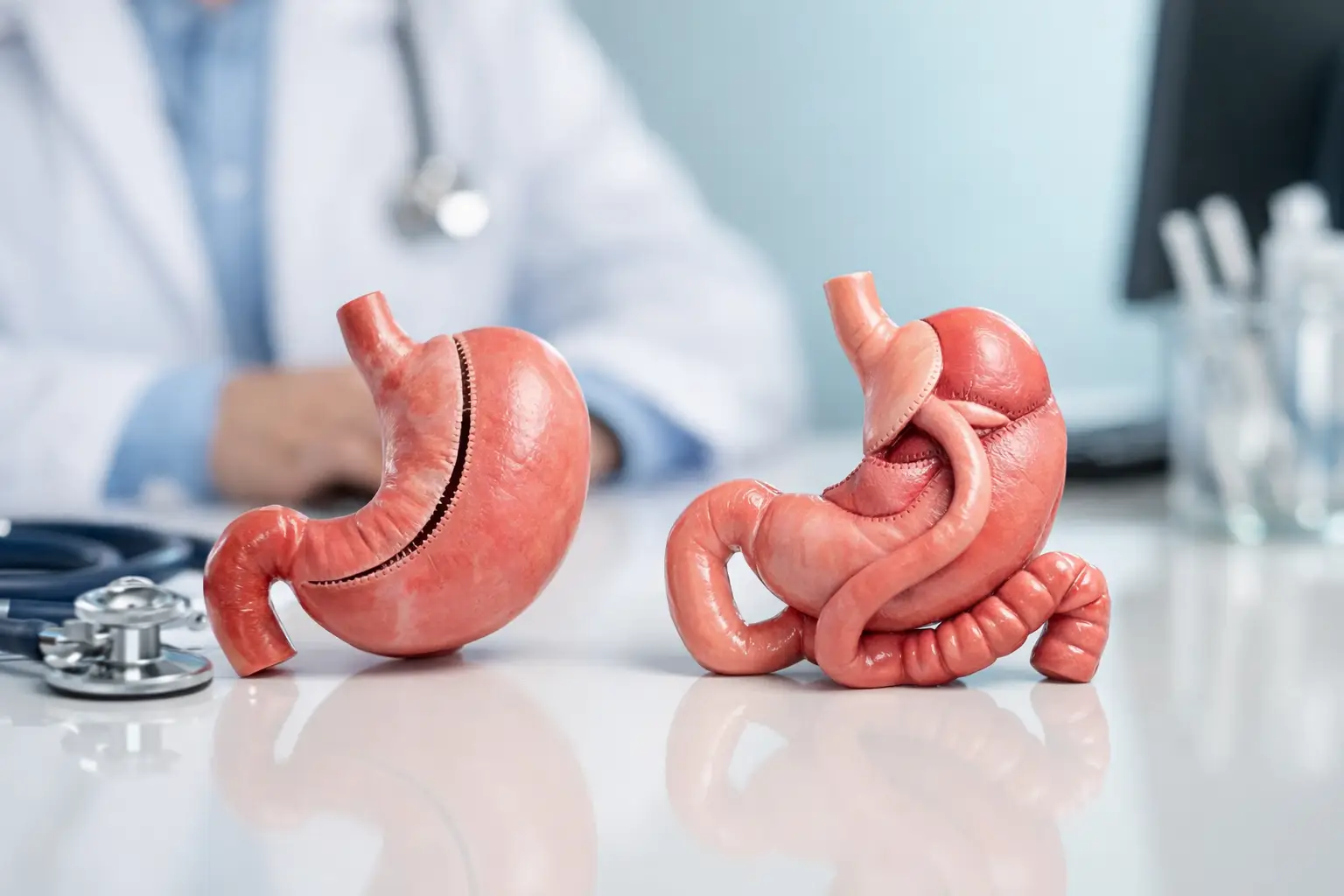
Sleeve vs bypass for reflux
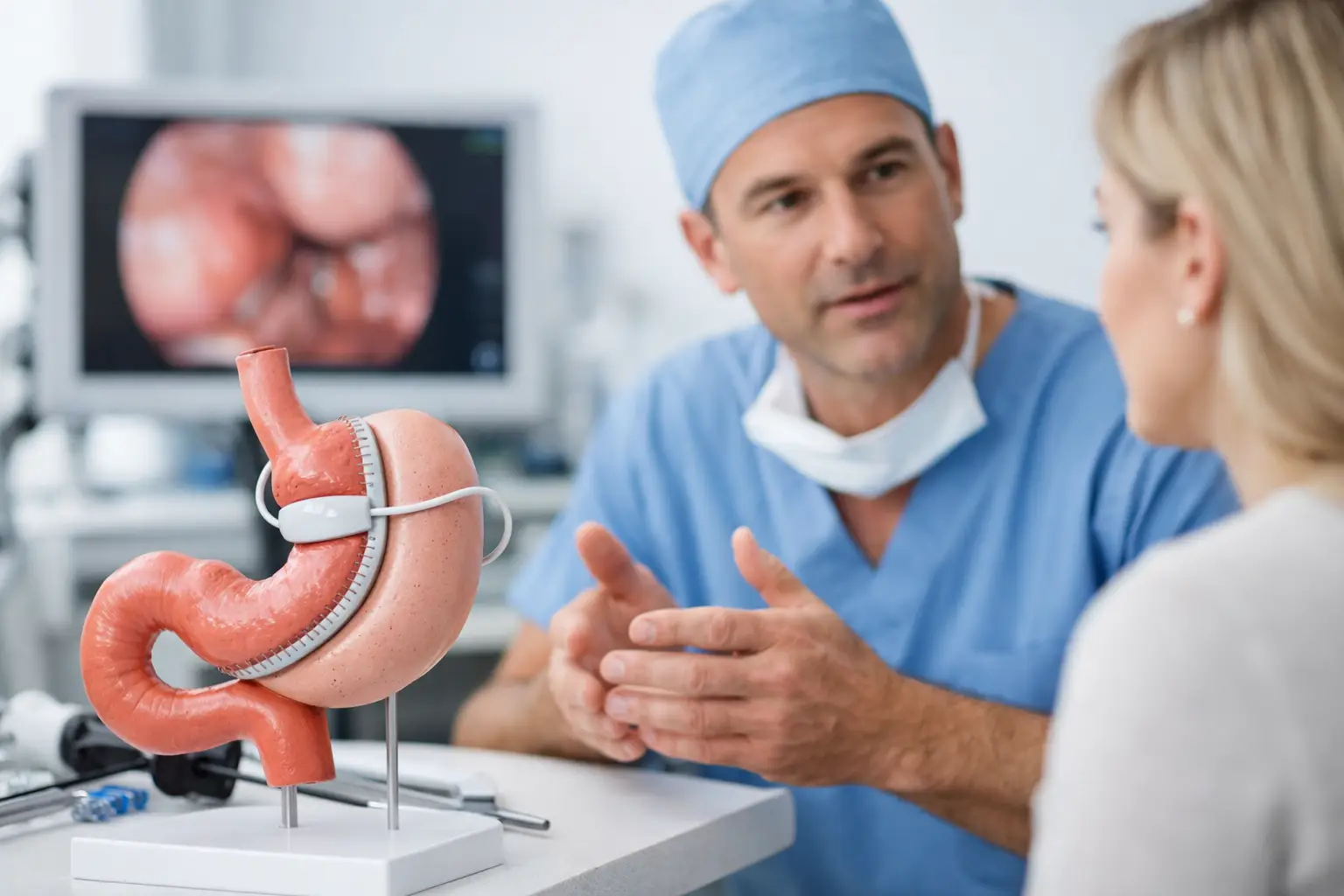
Gastric sleeve
The gastric sleeve remains one of the most requested procedures because it is effective, widely performed and technically straightforward in experienced hands. It reduces stomach volume and supports strong weight loss, which can improve many obesity-related symptoms.
But reflux is the trade-off that deserves honest discussion. In some patients, the sleeve can increase pressure within the newly shaped stomach tube and make acid reflux more likely. In others, existing reflux becomes more noticeable after surgery. If there is an untreated hiatus hernia, that can also contribute.
This does not mean sleeve surgery is wrong for everyone with any history of heartburn. A patient with very mild symptoms, normal investigations and a clear understanding of the risks may still be a reasonable candidate. The problem is assuming that because the sleeve is common, it is automatically the safest reflux option. It often is not.
Roux-en-Y gastric bypass
Gastric bypass is generally the stronger option when reflux is established. It creates a small gastric pouch and reroutes part of the digestive tract, which usually reduces acid exposure into the oesophagus. For patients with troublesome reflux, this can be a major advantage.
Bypass also provides excellent weight-loss and metabolic results, so it is not a compromise procedure. It is often the operation that gives patients both meaningful weight loss and relief from symptoms that have been affecting daily life for years.
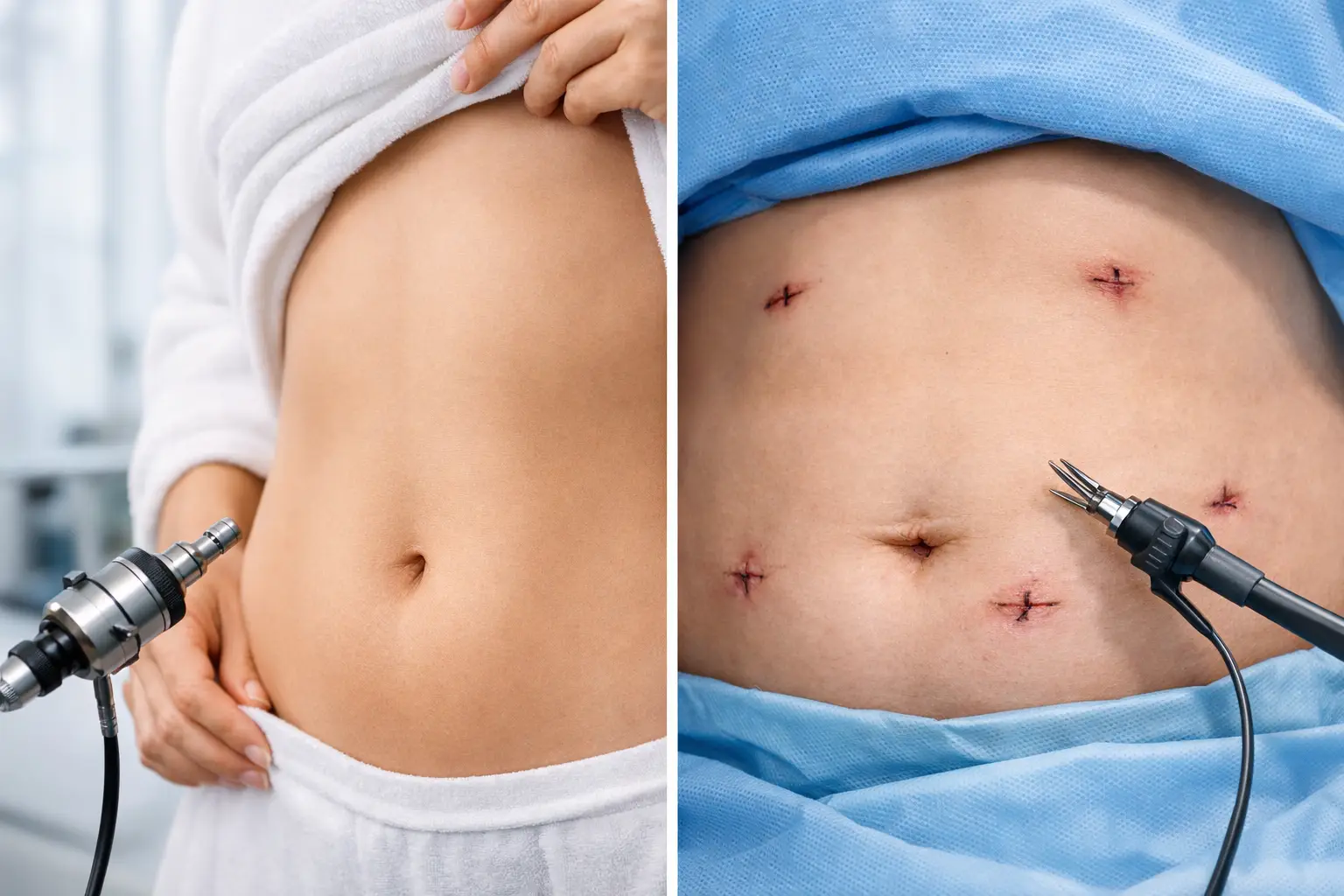
There are, of course, trade-offs. Bypass is more anatomically complex than sleeve surgery. Patients need to commit to lifelong supplementation, follow dietary guidance closely and attend follow-up. For the right patient, those responsibilities are worth it. But they still need to be understood clearly before moving forward.
Mini gastric bypass
Mini gastric bypass can also work well for weight loss, but when reflux is the central issue, the conversation becomes more nuanced. Some patients do well, while others may be at risk of bile reflux, which is a different problem from acid reflux and can be difficult to tolerate.
That does not make mini gastric bypass a poor procedure overall. It simply means that if your main question is reflux control, your surgeon may lean more strongly towards Roux-en-Y gastric bypass depending on your anatomy and symptoms.
When a sleeve can still be appropriate
There are situations where a sleeve may still be considered despite mild reflux. If investigations are reassuring, symptoms are infrequent, and a small hiatus hernia can be repaired at the same time, some surgeons may still regard sleeve surgery as reasonable.
What matters is honest consent. You should know that reflux may improve with weight loss, stay the same, or worsen after a sleeve. If your priority is avoiding reflux problems as much as possible, bypass usually gives more reassurance.
This is why the best consultations are specific. Not just “Which operation is best?” but “Which operation is best for my reflux history, my scans and my long-term goals?”
Best bariatric surgery for reflux after a previous sleeve
If you already had a gastric sleeve and now struggle with reflux, you are not alone. This is one of the most common reasons patients look into revisional bariatric surgery. Some develop new reflux after sleeve surgery, while others find that mild symptoms become much more disruptive over time.
In many of these cases, conversion from sleeve to Roux-en-Y gastric bypass is the most effective revisional option. It can address both ongoing reflux and weight-related concerns if weight loss has slowed or regain has started.
Before revision, your team may recommend endoscopy, imaging and a full symptom review to understand whether the issue relates to sleeve shape, narrowing, a hernia, inflammation or another anatomical factor. Revision should never be rushed, but when it is clearly indicated, it can make a significant difference to comfort and quality of life.
Questions your surgeon should answer clearly
If reflux is part of your decision, you should leave your consultation with clear answers. Ask whether your symptoms suggest acid reflux, whether a hiatus hernia is suspected, what operation is likely to help most, and what the plan would be if reflux persisted afterwards.
You should also ask what testing is needed before surgery and whether your medication history changes the recommendation. Patients often feel calmer once they understand that procedure choice is being based on evidence from their own case, not a standard package.
For international patients, that clarity matters even more. Travelling for surgery feels far more manageable when pre-op checks, hospital scheduling, hotel stays and follow-up are all explained in plain language. At Bridge Health Travel, that step-by-step support is a big part of helping patients feel safe enough to make a confident decision.
The safest way to think about procedure choice
The safest mindset is not to chase the quickest route to surgery. It is to choose the operation that solves the biggest problem without creating a new one you could have anticipated.
If reflux is frequent, requires regular tablets, wakes you at night or has been confirmed on testing, gastric bypass is usually the front-runner. If symptoms are mild and your assessment is reassuring, sleeve surgery may still be discussed, but it should be discussed carefully. If you already have a sleeve and reflux is now affecting your life, revisional bypass is often the treatment that deserves serious attention.
A good bariatric plan should make you feel informed rather than pressured. The right team will explain the trade-offs, arrange the right checks and tell you honestly when the more popular operation is not the better operation for you.
When patients ask about the best bariatric surgery for reflux, they are often really asking a deeper question: which option gives me the best chance of losing weight without living with constant discomfort afterwards? That is exactly the right question to ask, and it deserves a tailored answer built around your symptoms, your anatomy and the kind of support you want around you from the first consultation to the months after surgery.