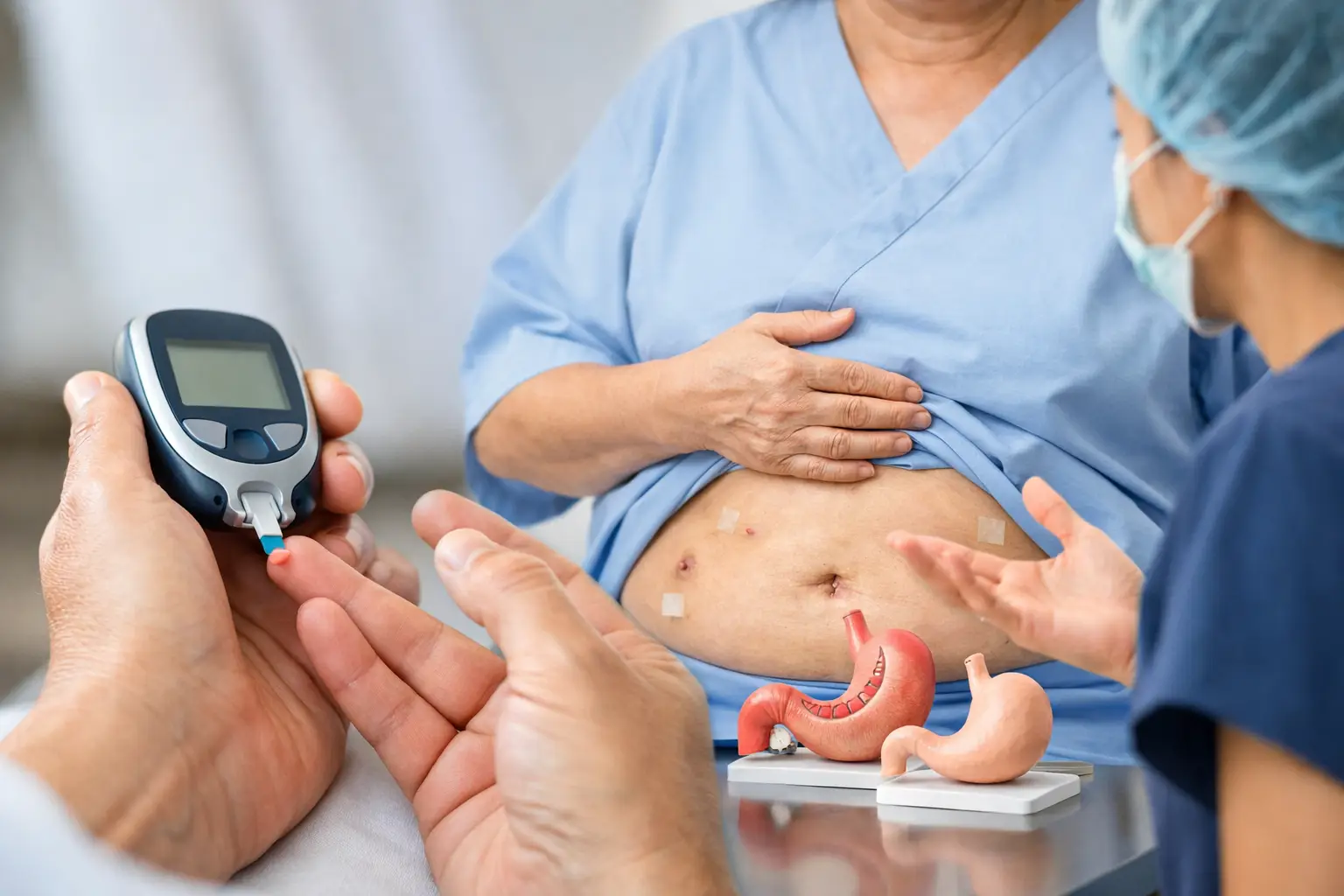
For many people, the most urgent question is not the number on the scales. It is whether life with type 2 diabetes might finally become easier. If you are asking can diabetes improve after bariatric surgery, the short answer is yes – often significantly – but the full answer depends on the type of diabetes, the procedure, and what happens after surgery.
Bariatric surgery is not simply about eating less. It changes hormones, insulin sensitivity, appetite signals, and the way the body handles glucose. That is why many patients see blood sugar improve within days or weeks, sometimes before major weight loss has even happened. For someone who has spent years juggling medication, diet plans, energy crashes and worry about long-term complications, that can be a very meaningful shift.
Can diabetes improve after bariatric surgery in real terms?
In real clinical terms, improvement can mean several different things. Some patients reduce their medication. Some come off insulin. Some achieve normal or near-normal blood sugar levels for a period of time, which may be called remission. Others still have diabetes after surgery, but it becomes easier to manage and less aggressive.
That distinction matters because surgery is powerful, but it is not magic. It does not guarantee a permanent cure. A careful team should be honest about that. The goal is usually substantial metabolic improvement and lower long-term risk, not a promise that diabetes will disappear forever.
Type 2 diabetes is the condition most likely to improve after bariatric surgery. This is especially true in people who have had diabetes for a shorter time, still make some of their own insulin, and have significant excess weight. If someone has type 1 diabetes, surgery may help with weight and insulin requirements, but it does not reverse the underlying condition.
Why blood sugar can improve so quickly
One of the more surprising things for patients is how soon change can begin. It is easy to assume diabetes improves only because of weight loss over many months. Weight loss absolutely plays a major role, but it is not the whole story.
Procedures such as gastric bypass and sleeve gastrectomy affect gut hormones involved in insulin release and appetite regulation. The body may start responding to insulin more effectively quite soon after surgery. Food intake also changes immediately, which reduces the glucose load the body has to manage. In some patients, fasting blood sugar starts improving during the early recovery period.
This early effect is one reason bariatric surgery is often described as metabolic surgery as well as weight-loss surgery. The operation is changing more than stomach size. It is influencing the whole system that governs hunger, blood sugar and insulin action.
Which bariatric procedures help diabetes most?
Different operations can improve type 2 diabetes, but they do not all work in exactly the same way or to the same degree.
Gastric bypass has long been associated with strong diabetes outcomes. Because it changes both restriction and nutrient flow through the digestive tract, it tends to have a pronounced hormonal and metabolic effect. Mini gastric bypass can also produce very strong blood sugar improvements in suitable patients.
Gastric sleeve is another effective option and is widely chosen because it offers substantial weight loss with a simpler digestive rerouting than bypass procedures. Many patients with type 2 diabetes do very well after sleeve surgery, particularly when their diabetes has not been present for decades.
The best procedure is not simply the one with the highest remission figures on paper. It depends on your BMI, eating pattern, reflux history, medication use, previous surgery, and the opinion of the bariatric surgeon and medical team. A good recommendation is always individual, not one-size-fits-all.
Who is most likely to see remission or major improvement?
If you want the honest answer to can diabetes improve after bariatric surgery, it helps to look at the factors that make strong results more likely.
Patients tend to do better when type 2 diabetes has been diagnosed more recently, when they are not on very high doses of insulin, and when pancreatic function is still reasonably preserved. Younger age can help, though older patients may still benefit a great deal. Greater weight loss after surgery usually improves the odds of sustained control.
On the other hand, long-standing diabetes can be harder to fully reverse. If the pancreas has been under strain for many years, the body may not recover enough insulin function for remission. Even then, surgery may still reduce medication needs, improve HbA1c, and lower the risk of complications affecting the heart, kidneys, nerves and eyes.
That is often an important point for patients who feel discouraged by the word remission. Better control still matters. Fewer medicines, steadier blood sugar and reduced health risk are valuable outcomes in their own right.
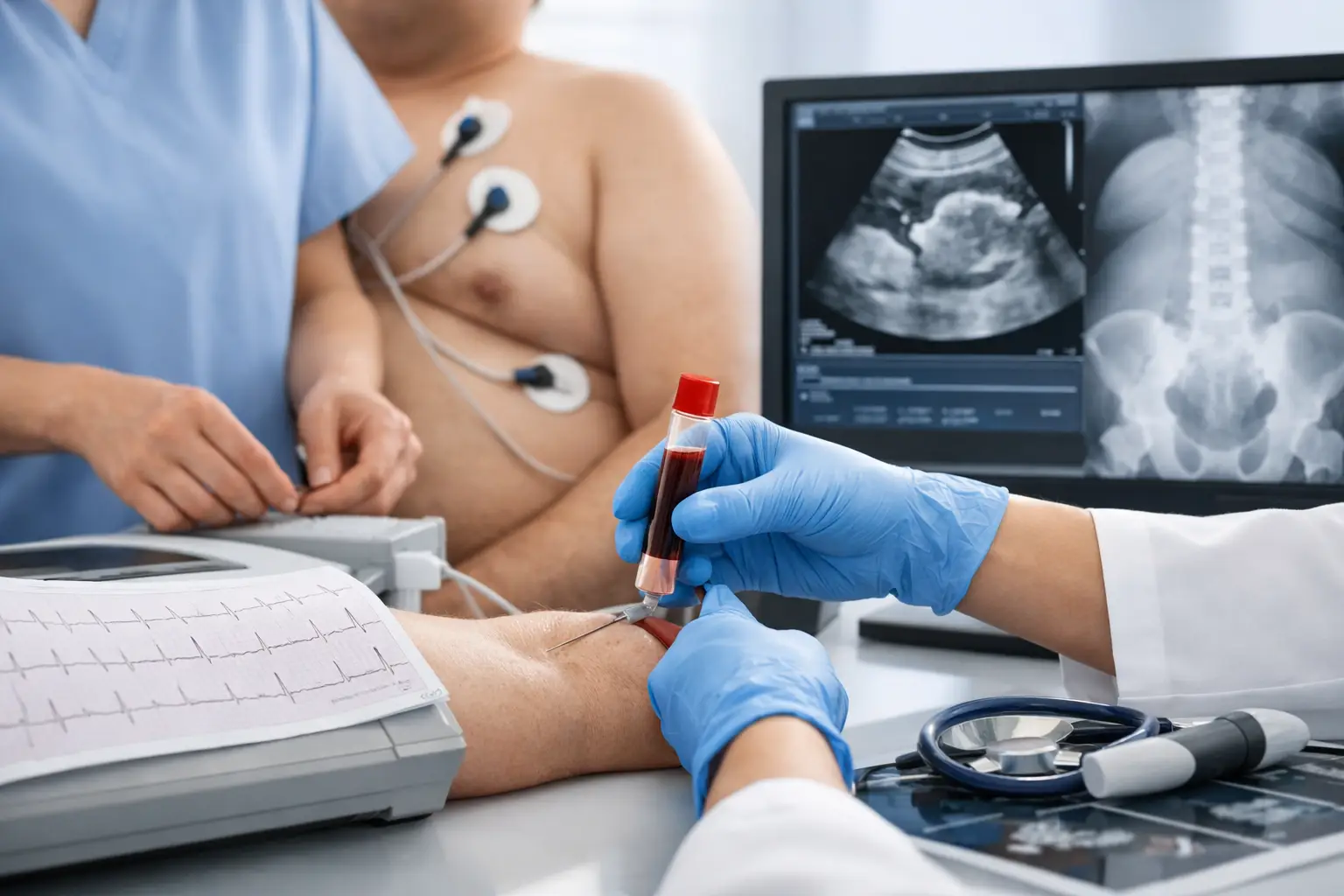
What results look like after surgery
Some people leave hospital already using less diabetes medication than before. Others need a more gradual adjustment over weeks and months as weight drops and eating patterns stabilise. Medication should never be changed casually after surgery. Blood sugars can shift quickly, and this needs proper medical oversight.
Over the first year, many patients see a marked improvement in HbA1c, fasting glucose and insulin resistance. Energy often improves as blood sugar becomes more stable. Daily life can feel less dominated by medication schedules, food cravings and the physical drag of obesity-related illness.
Still, results are not always linear. Some people have an excellent early response but need close follow-up later to keep that progress. If old eating habits return, weight regain can happen, and diabetes may come back or worsen again. This is why long-term aftercare matters as much as the operation itself.
The role of aftercare in keeping diabetes under control
Surgery creates the opportunity. Follow-up helps protect it.
Patients generally need ongoing blood tests, nutritional monitoring, supplement guidance and support with protein intake, hydration and meal structure. They also need realistic advice about activity, emotional eating and routine. Without that framework, it is easier to drift back into patterns that work against blood sugar control.
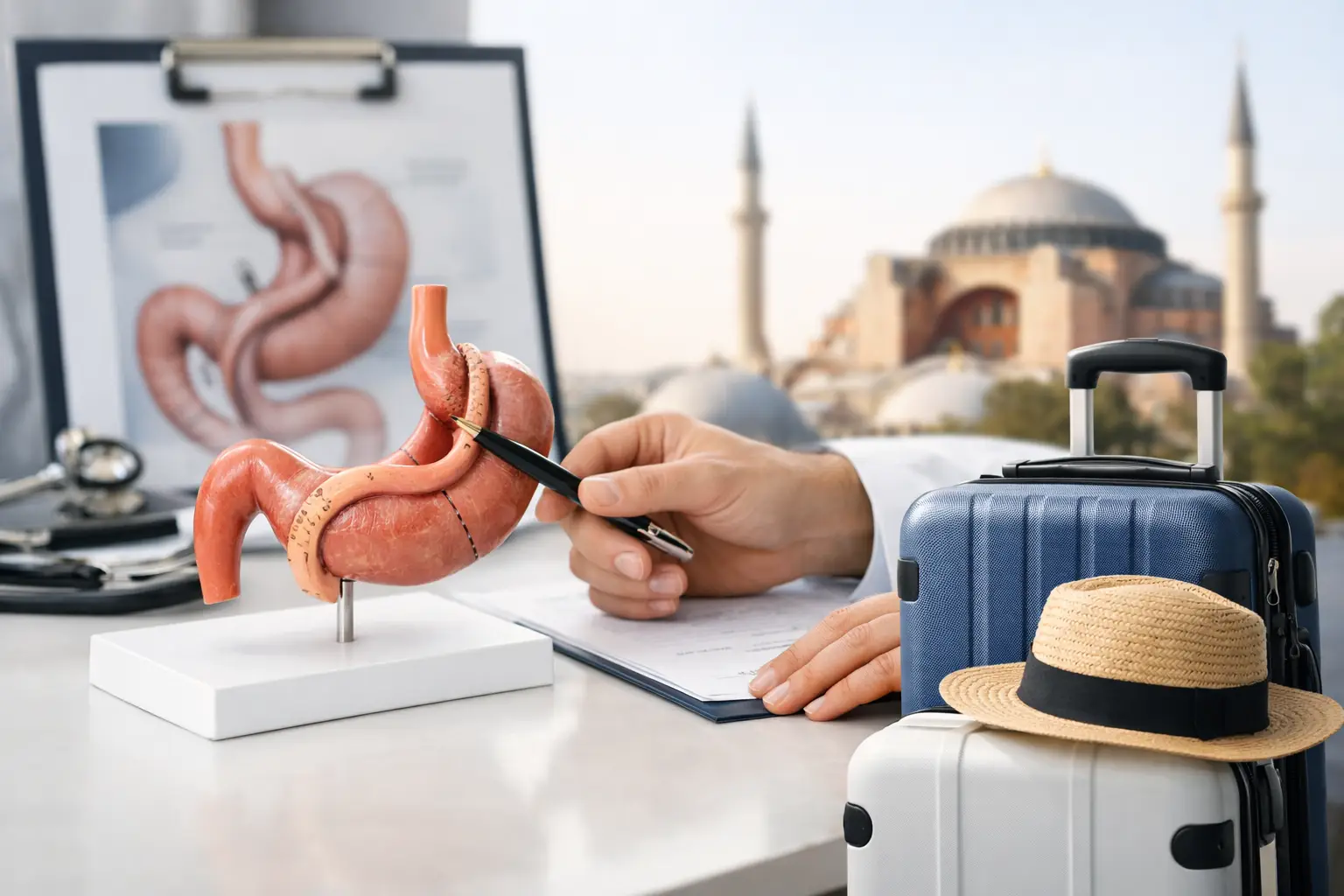
For international patients, this is one of the most overlooked parts of planning care abroad. The surgical procedure may take place over a few days, but the health changes unfold over months and years. That is why a coordinated pathway matters. Teams such as Bridge Health Travel place so much emphasis on organised testing, clear instructions and aftercare check-ins once you are back home.
A patient who feels supported is more likely to ask questions early, follow guidance properly and recognise when they need medication review or extra nutritional input. That does not just improve comfort. It improves safety and long-term outcomes.
Questions to ask before choosing surgery for diabetes
If diabetes is one of the main reasons you are considering bariatric surgery, ask direct questions. Which procedure is being recommended and why? How often does the surgeon treat patients with type 2 diabetes? What blood tests will be reviewed before surgery? How will diabetes medication be managed immediately after the operation? What aftercare is in place once you return home?
You should also be clear about the difference between hope and guarantee. A trustworthy team will explain likely benefits without overselling certainty. That kind of honesty is reassuring, not discouraging. It means your care is being planned around your health, not around marketing language.
A realistic but hopeful outlook
For the right patient, bariatric surgery can change the trajectory of type 2 diabetes. Blood sugar may improve quickly, medication needs may fall, and some people do reach remission. Just as importantly, many patients gain something less dramatic but deeply valuable – a condition that is easier to live with, easier to manage and less threatening to future health.
If you have been told for years to simply try harder, it can be a relief to learn that obesity and diabetes are not just matters of willpower. They are complex metabolic conditions, and surgery can be a clinically effective treatment when used carefully and supported properly.
The best place to start is with a full medical review and a team willing to look at the whole picture, including your diabetes history, your weight-loss goals, your anxieties, and what support you will need after the flight home. A calmer, healthier future often begins with that kind of clear conversation.