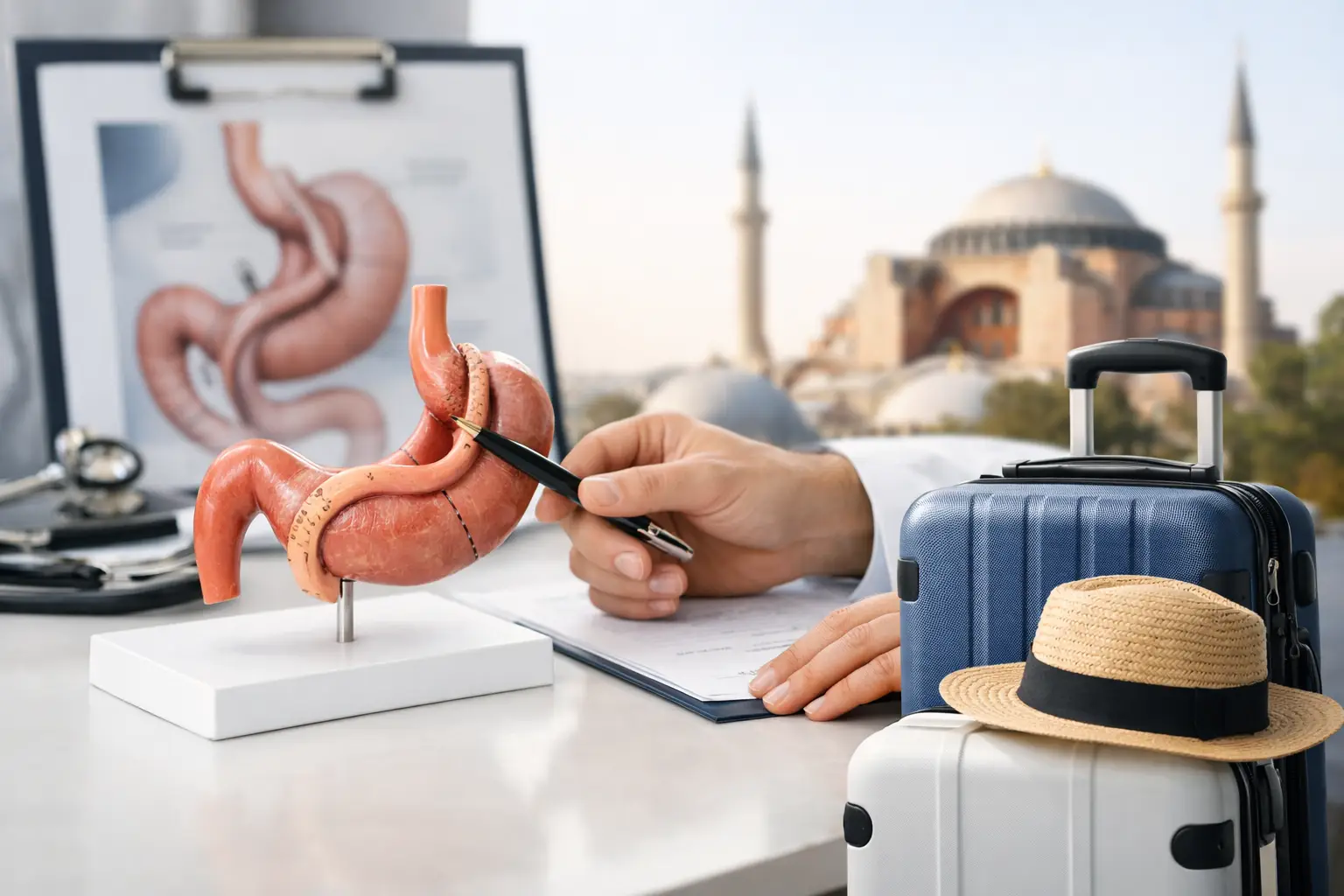
Most patients do not ask us first about the operation itself. They ask how long everything takes, when they can fly, how many days they need off work, and what recovery really looks like once they are back home. That is exactly why a guide to bariatric surgery timeline matters – it turns a stressful unknown into a clear sequence of steps you can prepare for.
For most people travelling for treatment, the timeline is not just medical. It is practical and emotional as well. You are arranging time away, speaking with family, budgeting, and trying to picture yourself in a hospital abroad while hoping you have made the right decision. A realistic timeline helps you feel in control and avoids the disappointment that can come from expecting too much, too soon.
Guide to bariatric surgery timeline: what to expect
The full journey usually begins weeks before your flight and continues for months after surgery. The exact pace depends on the procedure, your BMI, your medical history, and whether you need extra investigations before being cleared for theatre. A gastric balloon timeline looks different from a gastric sleeve or gastric bypass timeline, and revisional surgery often needs more planning than a first procedure.
Even so, most bariatric pathways follow the same broad stages: initial assessment, pre-travel preparation, arrival and testing, surgery, inpatient recovery, return to your hotel, flight home, then structured aftercare. Knowing that sequence helps you focus on one stage at a time rather than worrying about the entire process in one go.
Before you travel: the planning stage
This stage often lasts anywhere from a few days to several weeks. Some patients are ready to book quickly because they have already researched procedures for months. Others need more time to compare options, ask questions, or discuss the decision with a partner.
At this point, you would usually share medical information such as height, weight, age, previous operations, medications, and any conditions like reflux, diabetes, sleep apnoea, or high blood pressure. If you have had previous bariatric surgery, that will affect both the surgical recommendation and the timeline. Revisional cases can require older operation notes or extra imaging, which can slow things slightly.
Once a surgeon has reviewed your details, you can move into scheduling. This is also when patients start planning practical details such as annual leave, childcare, and whether a companion will travel with them. If you are coming from the UK or Ireland, many people aim to keep the trip as simple as possible by blocking out enough recovery time before returning to normal routines.
In some cases, you may be asked to start a pre-op diet before travel. This is especially common for sleeve and bypass patients. The goal is not crash dieting for the sake of it. It is to reduce liver size and improve surgical access, which supports safety in theatre.
Arrival in hospital and pre-op tests
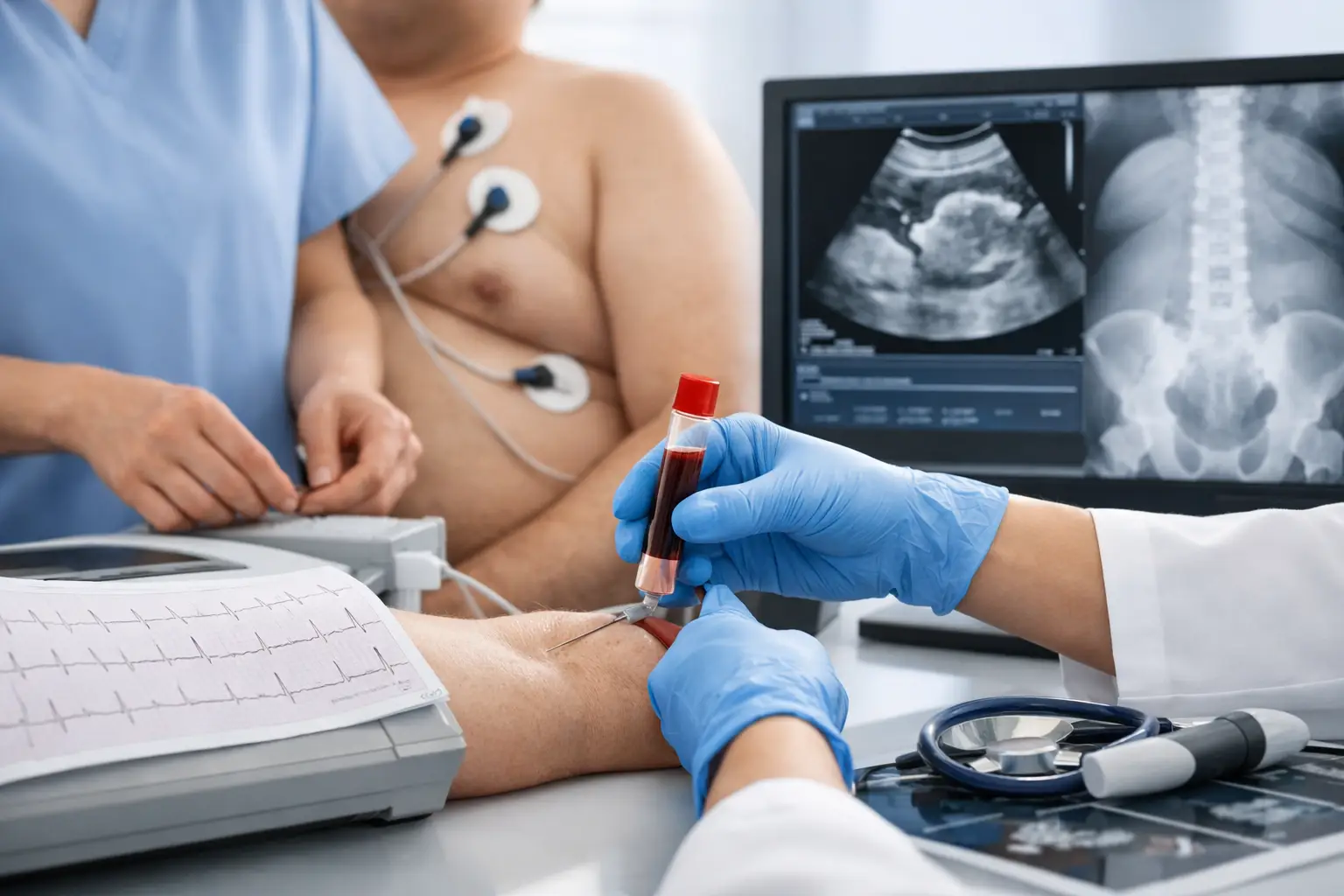
Once you arrive, the medical part becomes much more structured. Most patients have testing on the day of arrival or shortly afterwards. This commonly includes blood tests, ECG, and imaging such as chest X-ray or abdominal ultrasound, depending on the hospital protocol and your clinical picture.
This part of the timeline is important because it is where final suitability is confirmed. Even if everything has looked straightforward beforehand, a responsible team does not skip proper checks. Occasionally, these tests uncover something that needs a closer look. That can mean a short delay, a change in surgical plan, or, more rarely, advice not to proceed. Patients understandably find that unsettling, but it is a sign of safe practice, not poor planning.
You will also usually meet the surgeon and anaesthetic team, go over consent, and have a chance to ask final questions. By this stage, most people feel a mixture of relief and nerves. That is normal. Clear explanations and a well-organised admission process make a real difference here.
Surgery day and the first 48 hours
On surgery day, the procedure itself may only take one to a few hours depending on the operation. What matters more to most patients, though, is the first day afterwards. This is when you are waking up, getting mobile, managing discomfort, and beginning to understand how different your body feels.
For gastric sleeve, gastric bypass, and mini gastric bypass patients, early mobilisation is a standard part of recovery. You will be encouraged to walk as soon as it is safe to do so. This helps reduce the risk of complications and supports circulation. You may also have fluids introduced gradually, according to the surgeon’s protocol.
Discomfort varies. Some patients describe pressure, wind pain, tiredness, and a tight feeling in the abdomen more than sharp pain. Others feel surprisingly comfortable but very fatigued. There is no prize for recovering in the exact same way as someone else. Your age, fitness, procedure type, and pain tolerance all influence the first 48 hours.
During your hospital stay, regular checks matter. Surgeon reviews, nursing observations, fluid guidance, and support with walking all help build confidence before discharge. This is also the stage when anxious patients begin to realise they are not expected to manage alone.
The in-country recovery period
Most international bariatric patients do not fly home immediately after discharge. There is usually a short hotel recovery period first, allowing time for further review and ensuring you are progressing well before travel. That gap is useful medically, but it also helps emotionally. Hospital can feel intense. A quieter setting often gives patients space to rest and adjust.
This period is usually when the new routine starts to feel real. You are sipping fluids carefully, monitoring how much you can manage, walking a little more each day, and getting used to a smaller stomach or altered digestive pathway. Appetite can be very low at first, which some patients find reassuring and others find strange.
It is also when questions come up. Am I drinking enough? Is this pain normal? Why am I tired? Good coordinator-led support matters here because recovery is not just about what is clinically normal, but whether you understand what you are experiencing. Bridge Health Travel is built around that part of the journey – practical coordination paired with responsive reassurance.
Flying home and the first two weeks after surgery
Most patients feel ready to go home within several days, but that does not mean they feel fully recovered. Travel day can be tiring. You may be walking more than expected through the airport, sitting upright for long periods, and trying to maintain hydration while staying comfortable.
The first week at home is often quieter than people expect. Energy can dip. You may sleep more, move more slowly, and feel emotional for no clear reason. That does not automatically mean something is wrong. Surgery, travel, anaesthetic, and a major change in intake can all affect mood and stamina.
During the first two weeks, the main focus is usually hydration, prescribed supplements if advised, gentle movement, and following the staged diet exactly as instructed. This is not the time to test your limits. If your plan says fluids only or a purée stage, there is a reason for it. Healing tissues do better when patients resist the temptation to move ahead too quickly.
Weeks three to six: recovery becomes more practical
This is often the stage when patients want to know whether they are back to normal. The honest answer is that normal starts to return, but it is a new normal. Many people are walking more comfortably, doing light daily tasks, and noticing early weight loss. Clothes may feel different. Swelling settles. Confidence usually improves.
At the same time, this is a learning period. Eating habits need structure. Fluids and meals need separation. Protein matters. Some foods go down easily, while others feel unexpectedly difficult. If you have had a bypass, you may also be learning how your body reacts to sugar or richer foods.
Work return varies. Desk-based roles may be manageable sooner than physically demanding jobs. If your role involves lifting, long shifts, or constant movement, you may need more time. This is one of the biggest timeline mistakes patients make – comparing their recovery with someone whose job and operation were completely different.
Long-term milestones in a bariatric surgery timeline
By three months, many patients feel noticeably better in themselves. Weight loss is often well established, mobility may have improved, and conditions such as joint pain or poor stamina can begin to ease. Still, this is not the finish line. The early months reward compliance, but long-term success depends on habits that continue after the excitement of surgery fades.
At six months and one year, the timeline becomes less about healing and more about adaptation. You are not just recovering from an operation then. You are living with its effects. Follow-up matters because plateaus, food tolerance issues, reflux, constipation, vitamin deficiencies, or emotional adjustments can appear later rather than earlier.
That is why aftercare should never be treated as an optional extra. A well-managed timeline includes support after you have left hospital and after you have left the country. For international patients in particular, that continuity can make the difference between feeling abandoned and feeling properly looked after.
When the timeline changes
No responsible guide to bariatric surgery timeline should pretend every case runs perfectly to schedule. Sometimes blood results need repeating. Sometimes a patient arrives with a cough or infection and surgery needs postponing. Sometimes recovery is smooth but slower than expected.
That does not mean the process has failed. It means real medicine is being practised. The safest teams do not force a timeline when your body is asking for a different one. It can be frustrating, especially if you have arranged time off and flights, but flexibility is part of safe bariatric care.
If you are considering surgery abroad, ask not only how quickly you can be booked, but what support exists if something does not go exactly to plan. Fast access is helpful. Calm, competent coordination is better.
The best timeline is not the shortest one. It is the one that gives you enough space to prepare properly, recover safely, and come home feeling supported rather than rushed.